Related articles: Managing immunopathology, Science behind immunopathology

Table of Contents
Immunopathology
ImmunopathologyA temporary increase in disease symptoms experienced by Marshall Protocol patients that results from the release of cytokines and endotoxins as disease-causing bacteria are killed. (often abbreviated to IP) is what patients experience when they fight an infection. In the context of the Marshall Protocol, immunopathology refers to an increase in one's present symptoms of inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue., or a return of previous inflammatory symptoms. This is caused by cytokinesAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. and endotoxins being released from dying bacteria. Occasionally, immunopathology will consist of a new symptom or abnormal lab value due to the occurrence of subclinical inflammation that has been revealed by the Marshall Protocol (MP). Immunopathology is a necessary part of recovery for most patients. The amount of immunopathology a patient experiences on the Marshall Protocol (MP) is correlated with disease severity. Patients who are less sick will have comparatively less strong immunopathology.
Immunopathology is sometimes used synonymously with “herx” or the “Jarisch-Herxheimer reaction.”
Note that three forms of immunopathology are particularly life-threatening and should be handled with an abundance of caution: cardiac immunopathologyAn exacerbation in symptoms of the heart muscle. Requires careful management by physicians., neurological immunopathologyA temporary exacerbation of neurological symptoms due to bacterial death. Requires careful management by physicians., and respiratory immunopathologyA temporary exacerbation in symptoms of the lungs due to bacterial death. Requires careful management by physicians..
What is immunopathology?
Immunopathology is one's immune system reaction. Symptoms of immunopathology are unique to a patient and can include: fatigue, muscle weakness, rash, headache, photosensitivityAbnormal sensitivity to sunlight and bright lights. Also referred to as "sun flare" or "light flare.", pain anywhere, numbness, nausea, diarrhea, constipation, ringing in the ears, toothache, sinus congestion, nasal stuffiness, fever/chills, flu-like bodyache, cough, irritability, depression, sleep disturbances and “brain fogThe loss of intellectual functions such as reasoning; memory loss; and other neurological abilities that is severe enough to interfere with daily functioning..”
Any symptom, including abnormal lab results, that correlates with MP therapy is most likely due to immunopathology. Patients who are less sick will have comparatively less strong immunopathology.
The increase in symptoms due to immunopathology typically begins 1-24 hours after the minocycline dose and usually dissipates 12-24 hours before the next antibiotic dose. Many patients find that the reaction is strongest on the second day.
As opposed to the disease itself, which progresses over the course of decades, immunopathology symptoms usually flare quickly. However, dramatic waxing and waning of immunopathology does not always happen. An increase in symptoms may be constant.
Immunopathology is sometimes mistaken for an allergy to a MP antibiotic.
A number of strategies are available for managing immunopathology.
Expected symptoms of immunopathology
When bacteria are killed, endotoxins and cytokines are released at the site of the infection. This contributes to a sense that one's original disease is getting worse. In fact, the increase in symptoms is only temporary. Although these symptoms may be similar to one's disease, unlike disease symptoms, they are a sign that something is being accomplished: the Th1 pathogensThe community of bacterial pathogens which cause chronic inflammatory disease - one which almost certainly includes multiple species and bacterial forms. are being killed.
The immunopathological reactionA temporary increase in disease symptoms experiences by Marshall Protocol patients that results from the release of cytokines and endotoxins as disease-causing bacteria are killed. is caused by release of toxins and the apoptosis (die off) of infected cells. People with effective detoxification and elimination systems may not experience significant aggravation of symptoms. Some of my patients just experience gradual improvement in health. Others experience mild loss of stamina, periodic night sweats or emotional swings.
I firmly believe that Th1 patients no matter what their diagnosis react similarly.
I would suggest evaluating present condition with that which was present prior to starting the MP. Most patients with a diagnosis of borrelia have significant physical or cognitive loss and have received other therapies prior to them starting the MP. Some of these therapies can result in delayed or reduced immunopathological reactions.
Greg Blaney, MD
As evidenced by high rates of depression and anxiety in the population at large, the brain itself is a frequent site of chronic bacterial infection. One of the challenges of having neurological immunopathology is a lack of awareness about the role infection and immunopathology play in one's mood, cognitive abilities, and ability to think clearly. It is very common for patients with neurological immunopathology not to recognize that their recovery will involve the temporary exacerbation of these types of symptoms. One's life events play a role in, say, depression, but often enough they are not the driving force behind it.
Along with neurological immunopathology, cardiac immunopathology and respiratory immunopathology are potentially life-threatening. Patients who have, or worry that they may have, these symptoms should work particularly closely with their physician and proceed on the MP cautiously.
Unexpected symptoms of immunopathology
The MP can't create new inflammation because it can't make bacteria appear where there weren't any before. The presence of new symptoms is a clear indication that bacteria are being targeted in areas of the body not known to be infected. In the absence of undergoing some kind of curative therapy like the MP, it seems probable that these sites of sub-clinical infection would in time be part of the disease process.
If extra Benicar reduces a symptom, one can be sure it is due to immunopathology. But, lack of response to Benicar does not rule out immunopathology. Palliative medication may reduce symptoms of immunopathology also.
Necessity of immunopathology
Immunopathology is not a “side effect” of the MP – not in the traditional sense anyway. Also, the MP does not “cause” an exacerbation of disease symptoms. Patients are hardwired to equate symptoms with disease, but what many do not realize is that all disease symptoms are the result of an immune system response.
A rise in intensity of symptoms is not a sign that the disease process is advancing, but an indication that the immune system is active and killing bacteria. If a person gets infected with a virus, the rise in symptoms he or she displays is not caused by the virus, but the response of the immune system to the virus. The symptoms of food poisoning including diarrhea and vomiting are very unpleasant, but are extremely effective in rapidly eliminating toxins.
The Jarisch-Herxheimer response, a term which is sometimes used interchangeably with immunopathology, has been documented as necessary to recovery in over 10 diseases, to say nothing of evidence supporting the MP's effectiveness.
Based on everything we know about the way the bacteria have parasitized the immune system, and the way they affect the body's molecular chemistry, I am sad to say that it seems 'no pain, no gain.'
I suspect we will find some palliative techniques as time goes by, especially for pain, but the starting point is relatively unpalatable, I am afraid. This is, of course, one of the reasons why nobody has been able to develop a therapy until now. Until you understand the pathogenesis, there is no way that 'no pain, no gain' makes any sense. But when you understand how the bugs are wreaking their havoc - it all becomes crystal clear.
Trevor Marshall, PhD
A potent anti-inflammatory, Benicar should palliate negative symptoms and minimize any tissue damage caused by the disease process.
Assessing immunopathology
Immunopathology is necessary for making progress on the MP. Throughout the course of one's treatment, the goal is to generate a tolerable level of immunopathology. But how does one determine if immunopathology is tolerable or intolerable?
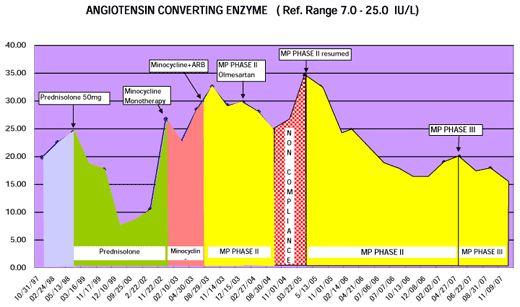
Using lab tests to track immunopathology
With chronically ill patients, it is common to disassociate from one's feelings and therefore it can be difficult to determine the sometimes subtle shifts associated with Herx reactions…. My use of lab tests is to help determine pace of therapy especially if degree of Herx reaction is difficult for patient to interpret.
Greg Blaney, MD
Abnormal lab work or ECG tracing may reveal unacceptable “silent” immunopathology. In that case, monitor these signs regularly and use them as a guide to gauge pace of therapy.
Other ways to assess immunopathology
Even for diseases that have ideal measures for tracking immunopathology, it is sometimes possible to have a flare in symptoms and not know why. This is particularly true for patients whose diseases have a strong mental component and have trouble thinking critically about their illness. Sometimes the onset of uncomfortable symptoms simply cannot be explained, only managed. Other times though, it is a factor within a patient's control. These questions might help patients gain insight into why they feel worse.
| Issue | Questions |
|---|---|
| Symptoms | Has a signature symptom(s) gotten worse? Is a symptom new? Have symptoms reached a plateau approaching intolerable? Are familiar symptoms different? Has there been a window of change for the better? Have symptoms slowly been getting worse or are they constant? |
| Symptom severity | To what extent do my symptoms interfere with activities of daily living: dressing, eating, ambulating, toileting, hygiene, etc.? To what extent do my symptoms interfere with instrumental activities of daily living: shopping, housework, cooking, transportation, etc.? Do I need to keep track of my symptoms by using a symptom chart? |
| Light | Am I diligently avoiding light indoors and outside? Am I wearing my NoIRSpecial sunglasses worn by Marshall Protocol patients to block light. glasses or other glasses which protect against infrared? |
| Foods and medications | Have I changed the food or drink I consume? Am I eating regularly? When is the last time I have eaten? Do I need to eat now? |
| Non-MP medications | Has there been any change in non-MP medications, over the counter supplements? Do I need to take any palliative medications now? Am I weaning off immunosuppressive drugs like Prednisone too quickly? |
| MP medications | Is my Benicar dose due? How consistently have I been dosing Benicar? Is my minocycline dose due? Am I ramping too quickly? Do I need a change in my dosage schedule? |
| Environment | Have I been exposed to anything, which could exacerbate immunopathology: toxins, heat or climate changes, stress, etc.? Am I over-heated or not warm enough? |
| Expectations | Do I understand and accept my own limitations? Have I reassessed family and social obligations and expectations? Have I been clear with others about what I can or cannot do? |
| Unmet needs | Do I need to rest or sleep? Do I need some social contact by phone, private message, email etc.? Do I need some quiet time? Have I clearly asked for support and assistance where I need to, each time I need to? What can I do or ask for myself that will be helpful? What will make me feel relieved or comfortable? What can I do to pamper myself? |
| Activity | Have I avoided making commitments that are not necessary for recovery? Has there been a change in levels of physical or mental exertion? Have I recently gotten a massage or done stretching or yoga? |
| 25-D | Has my level of 25-D dropped in recent months to the point where my innate immune responseThe body's first line of defense against intracellular and other pathogens. According to the Marshall Pathogenesis the innate immune system becomes disabled as patients develop chronic disease. is becoming increasingly activated? |
| Asking for help | Have I posted on the MP forums and asked for help? Do I need to contact my doctor? |
Another way to look at immunopathology is to ask oneself this question: “If a well person suddenly came down with my symptoms today what would s/he feel like doing?”
Patients experiences
It is my observation and experience that the Herx is one of the most difficult things for people to understand. When symptoms “act up” they get the jitters - understandably, due to the years of disease and being so symptomatic. Many feel they are getting worse. … But when the symptoms do occur as they do with Herx - I have witnessed that symptoms begin to fade and then never re-appear.
Ms Dale, MarshallProtocol.com
Chance events or environmental factors may complicate correct analysis of immunopathology. Suppose my reading of symptoms should take into account that herx produces base symptoms plus vulnerabilities. Intensification of symptoms out of proportion to the usual herx pattern may result when chance events or environmental factors act on the vulnerability to potentiate herx signal. Thus complicating time series analysis greatly and leading to incorrect interpretation of signals.
Tgritton, MarshallProtocol.com






