Related articles: Managing immunopathology, Immunopathology

Table of Contents
Science behind immunopathology
When patients on the MP kill bacterial pathogens they experience a reaction called immunopathologyA temporary increase in disease symptoms experienced by Marshall Protocol patients that results from the release of cytokines and endotoxins as disease-causing bacteria are killed.. Immunopathology is an increase in one's present symptoms of Th1 inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue., or a return of previous Th1 inflammatory symptoms, that is caused largely by cytokinesAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. generated by the immune response and endotoxins released from dying bacteria. Occasionally, immunopathology will result in a new symptom or abnormal laboratory value (e.g., elevated creatinine, elevated liver enzymes, low white blood count, etc.). The occurrence of subclinical bacterial inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue. is due to olmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. 's activation of the immune system. Immunopathology appears to be a necessary part of recovery. The amount of immunopathology a patient experiences on the Marshall ProtocolA curative medical treatment for chronic inflammatory disease. Based on the Marshall Pathogenesis. (MP) tends to correlate with disease severity and bacterial load. Patients who are less sick will have comparatively less-strong immunopathology.
Immunopathology is sometimes used synonymously with the “Jarisch-Herxheimer reaction” or “herx.”
Many MP patients who have experienced prolonged periods of immunopathology have reached stages of significant improvement or remission. This supports the conclusion that immunopathology is a necessary result of chronic bacterial death, and a precursor to disease reversal. The MP is not unique in this regard. A number of other diseases and/or therapies generate immunopathological or immunopathological-like reactions.1) 2) 3)
Lab work and patient reports can be used to track clinical signs of immunopathology.
Competing models for immunopathology
According to a 2010 review by evolutionary biologist Paul Ewald, PhD, there are essentially three categories of explanations for immunopathology in chronic disease:4) - The immune system is exposed to environmental conditions to which the individual is not well adapted. One hypothesis within this category, often referred to as the hygiene hypothesis, proposes that new more hygienic environmental conditions have generated compositions of symbionts that differ from those to which humans have been adapted. - Infectious agents act as triggers of immunopathology by shifting the immune system into a self-destructive state. - Infectious agents cause collateral damage by virtue of persistent and ongoing infections.
Of the three , the third and final explanation is most consistent with the Marshall PathogenesisA description for how chronic inflammatory diseases originate and develop..
Symptoms of infection are caused by the body's response to microbes
A 2011 study, using a novel mouse model, showed that mice that were engineered to have a reduced innate immune responseThe body's first line of defense against intracellular and other pathogens. According to the Marshall Pathogenesis the innate immune system becomes disabled as patients develop chronic disease. to the common cold actually showed less – not more – airway inflammation and bronchoconstriction (airway spasm) following infection.5) According to the study's lead author:
In our study, we offer the first direct evidence that limiting the immune response reduces the manifestations of rhinovirus infection. In our model, cold-induced asthma flare-ups were caused by the body's immune response to the virus, not the virus itself. Chemicals produced by the immune system inflame cells and tissues, causing asthma symptoms such as cough and wheeze.
Marc B. Hershenson, M.D., ScienceDaily June 17, 2011
Even though it was conducted in a murine modelA model of disease which uses rats or mice to mimic human conditions., this work is relevant as it strongly suggests that symptoms of infection are due not so much to the infection but the body's response to it.
Molecular nature of immunopathology
In patients suffering from any of the Th1 diseasesThe chronic inflammatory diseases caused by bacterial pathogens., pulsed low-dose antibiotics and frequent administration of olmesartan (Benicar)Medication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. kill intraphagocytic and other pathogenic forms of bacteria. When bacteria die, endotoxins and inflammatory cytokines (signaling molecules) are released at the site of infection. Cells with a significant bacterial load will be destroyed along with the microbiotaThe bacterial community which causes chronic diseases - one which almost certainly includes multiple species and bacterial forms., and this adds to the immunopathology.
Cytokines
Related article: Innate immune response and Th1 inflammation
During immunopathology, cytokines, are elevated. Cytokines are released by the inflammatory process.
The release of cytokines appears to be essential for recovery after an infection. One study found that the cytokineAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. TNF-alphaA cytokine critical for effective immune surveillance and is required for proper proliferation and function of immune cells. was essential for the proper expression of acquired specific resistance following infection with Mycobacterium tuberculosis.7) 8) 9) For this reason among others, TNF-alpha inhibitors, drugs which suppress the cytokine, are contraindicated for MP patients.
Endotoxins
Endotoxins, sometimes referred to as lipopolysaccharides, are proteins associated with bacteria and bacterial communities (microbiota). When these bacteria are destroyed by the innate immune system, as will happen during the MP, endotoxins are released causing a spike in symptoms known as an immunopathological reactionA temporary increase in disease symptoms experiences by Marshall Protocol patients that results from the release of cytokines and endotoxins as disease-causing bacteria are killed..
The body responds to the presence of endotoxins by producing cholesterol10) and C-reactive protein,11) among other defense mechanisms.
In immunology, the term “LPS challenge” refers to the process of exposing a subject to a lipopolysaccharide that may act as a toxin. Injecting mice with LPS has been used as models for preterm labor,12) hyperactivity,13) lung injury,14) and periodontitis,15) to cite just a few examples.
<html> <!–
–> </html>
Exacerbation of symptoms
We need to change our paradigm from the existing one that symptoms are directly due to the pathogen or insult to the understanding that the symptoms and in fact clinical markers are due to the immune response. So instead of believing shingles erupts or herpes erupts or cystitis symptoms erupts when our immunity is depressed, we see these eruptions as an immune activation.
Of course, if there are factors suppressing immune function than these reactions will be ineffective long term. But our routine approach of suppressing symptoms when faced with an “acute illness” is likely promoting chronic problems.
Greg Blaney, M.D.
The increase in endotoxin and cytokines causes a corresponding increase in symptoms. Sometimes the symptoms are generalized and may include pain and fatigue. Other times symptoms occur at the site of infection. Patients with the lung disease sarcoidosis may notice that their coughing spells get worse. Those with psoriasis may notice a flare in their skin symptoms.
Cardiac, neurological, and respiratory immunopathologyA temporary exacerbation in symptoms of the lungs due to bacterial death. Requires careful management by physicians. should be of particular concern to healthcare providers as they can be life-threatening.
Occasionally, patients may notice new symptoms occurring in organs not known to be infected. The MP cannot create new infection, such symptoms are due to exacerbation of previous sub-clinical microbiota.
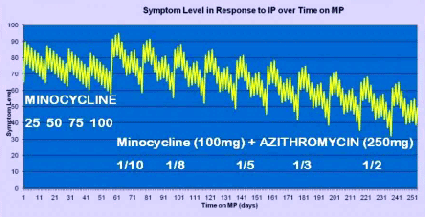
The strength of an immunopathological or herx reaction is associated with the severity of disease.16) 17)
Other examples of immunopathology
The Jarisch-Herxheimer reaction is similar if not identical to immunopathology. These reactions have been accepted as an indication of progress and, according to the literature, have been observed in at least ten different diseases and conditions:
- Borrelia infection21)
- tuberculosis24)
- leptospirosis25)
- Whipple disease26)
- sarcoidosis27)
- relapsing fever28)
Recovery from other infections and diseases also entails an immunopathological-like response:
- fever – Fever, a natural increase in one's body temperature, has been conserved during evolution through millennia, because of its advantage for host defense.30) Important immunological reactions are sped up by temperature, and some pathogens with strict temperature preferences are hindered.31)
- immune recovery uveitis – An intraocular inflammatory disorder originally described in individuals with human immunodeficiency virus (HIV) and inactive cytomegalovirus retinitis following highly active antiretroviral therapy (HAART). IRU can occur when immunosuppressed patients immune systems' become reinvigorated in HIV-positive or negative individuals.32)
- Graves disease – Rasul reported four cases of Graves' disease emerging in HIV patients on HAART.33)
- common cold (rhinovirus) – Another example of immunopathology can be observed in the body's response to the rhinovirus. The symptoms of the common cold, which is caused by the rhinovirus, are an indication that the human host is in the midst of an activated immune response. Researchers have shown that during the common cold, the expression of many genes associated with the immune response, including chemokines and antivirals, are altered.34) It's important to note that the rhinovirus doesn't exactly cause the immune response so much as trigger it. Similarly, olmesartan and MP antibiotics do not cause the immunopathological reaction so much as trigger it.
Immune reconstitution inflammatory syndrome (IRIS)
During IRIS, HIV/AIDS patients experience the worsening or onset of systemic inflammatory clinical signs and symptoms following treatment with highly active antiretroviral therapy (HAART). This syndrome results when HAART allows for partial recovery of the immune response. This causes renewed and exuberant host immunological responses towards opportunistic infectious agents, agents that the host accumulated during prior periods of immunosuppression.35)
A number of well-known readily cultured pathogens have been conclusively linked to IRIS: the herpes viruses, cytomegalovirus, hepatitis B and C, M. tuberculosis, Mycobacterium avium complex and Cryptococcus neoformans.36) However, many more microbes likely contribute to the reaction since AIDS clinicians do not yet have access to the metagenomic tools. Certainly, the existence of IRIS in culture-negative HAART patients suggests that more microbes may be present than the few that have already been isolated.37)
Interestingly, patients experiencing IRIS often “develop” autoimmune conditions as a manifestation of immune restoration. These include sarcoidosis and other granulomatous reactions,38) 39) diabetes mellitus, rheumatoid arthritis,40) systemic lupus erythematosus,41) Guillain–Barre syndrome,42) Graves disease43) and autoimmuneA condition or disease thought to arise from an overactive immune response of the body against substances and tissues normally present in the body thyroid disease.44) 45) This suggests that these patients accumulated microbes that are directly involved in the pathogenesis of these disease states.
In a 2009 study, Sun and Singh reviewed the existence of IRIS in non-HIV immunocompromised patients including solid organ transplant recipients, women during the postpartum period, neutropenic patients, and tumor necrosis factor antagonist recipients.46)
Immunopathology reveals disease
Given its pervasiveness across diseases, immunopathology belies the common assumption that feeling well is the same as being healthy.
In observing a set of worsening symptoms, patients and clinicians may be tempted to assume that the disease itself is worsening. Even a small number of researchers are mistakenly convinced that antibiotics cause or exacerbate chronic disease. The best example of this may be so-called “minocycline-induced lupus.”47) In fact, there is no reasonable mechanism, proven or theoretical, which explains how minocycline, the primary action of which is to block the 30s ribosome of bacteria, can cause lupus – or any other disease.48) Nor is there a mechanism by which olmesartan can cause porphyria cutanea tarda (a blood disorder) as was reported in a 2010 Journal of the European Academy of Dermatology and Venereology paper.49)
Edward L. Krawitt, M.D. has it right when he suggests the possibility that minocycline, “unmasks” autoimmune hepatitis.50)
In the same vein, an “allergic” reaction to minocycline or any of the other antibiotics formerly used with Olmesartan was invariably due to the immunopathological response generated by taking olmesartan (Benicar) and antibiotics.
Some Marshall Protocol patients have reported that the treatment appears to clinically reveal markers of latent infections.
My wife, Carol, who has been on the Marshall Protocol since 8/2003 with rheumatoid arthritis, suffered an eye condition over a year ago that doctors said looked very much like Trachoma. Trachoma is a third world eye infection caused by Chlamydia. The eye doctor asked her if she had travelled to a foreign country recently, and she had not. They were then forced to conclude that it was not Trachoma, although we strongly suspected that it was.
Phil, Bacteriality.com
Even olmesartan alone may reveal infection as a 2012 study by Mayo clinic researchers suggests.51) A study of 22 patients with diarrhea and taking standard doses of olmesartan showed that those symptoms improved upon discontinuation of the drug.
Immunopathology can be suppressed
One of the common instincts among researchers who study immunopathological type reactions is to suppress this reaction.52) Indeed, two German papers have noted that the Jarisch-Herxheimer reaction can be suppressed with the administration of different kinds of prednisolone, a powerful corticosteroidA first-line treatment for a number of diseases. Corticosteroids work by slowing the innate immune response. This provides some patients with temporary symptom palliation but exacerbates the disease over the long-term by allowing chronic pathogens to proliferate..53) 54)
However, one of the factors that may play a large role in the incidence and prevalence of chronic disease is that the immunopathological reaction is being systematically inhibited on a population-wide basis. There are a broad range of substances including prescription drugs, supplements, and foods that inactivate the innate immune response. These include, among many others:
Read more
- Depiction of the six stages of disease and recovery – prepared by Janet Raty
Related publications and presentations
[PMID: 11997718] [DOI: 10.1097/00005792-200205000-00005]
[PMID: 18600241] [DOI: 10.1038/eye.2008.204]
[PMID: 12604286] [DOI: 10.1054/jocn.2002.1129]
[PMID: 20415848] [PMCID: 2841832] [DOI: 10.1111/j.1365-2249.2010.04127.x]
[PMID: 21637773] [PMCID: 3102730] [DOI: 10.1371/journal.ppat.1002070]
[PMID: 18544042] [PMCID: 2612548] [DOI: 10.1111/j.1365-2567.2008.02865.x]
[PMID: 12852719]
[PMID: 15216471] [DOI: 10.1086/421522]
[PMID: 20377753] [DOI: 10.1111/j.1348-0421.2010.00203.x]
[PMID: 15198851] [DOI: 10.1179/096805104225004833]
[PMID: 19995880] [DOI: 10.1093/molehr/gap106]
[PMID: 18814846] [PMCID: 2692986] [DOI: 10.1016/j.bbi.2008.09.002]
[PMID: 16273282]
[PMID: 15218043] [DOI: 10.1177/154405910408300706]
[PMID: 15896248] [DOI: 10.1111/j.1365-2710.2005.00631.x]
[PMID: 6017505] [PMCID: 1841580]
[PMID: 606336] [PMCID: 1045450] [DOI: 10.1136/sti.53.6.389]
[PMID: 9610974] [DOI: 10.1016/s0736-4679(98)00011-0]
[PMID: 9846580] [DOI: 10.1038/4007]
[PMID: 15617845] [DOI: 10.1016/j.mehy.2004.09.011]
[PMID: 11516219] [DOI: 10.1054/mehy.2001.1277]
[PMID: 12827534] [DOI: 10.1007/s10096-003-0957-8]
[PMID: 11721494]
[PMID: 15246025] [DOI: 10.1016/j.autrev.2003.10.001]
[PMID: 12380884] [DOI: 10.4314/eamj.v79i2.8908]
[PMID: 20428100] [DOI: 10.1038/ki.2010.111]
[PMID: 16613288] [DOI: 10.1024/0040-5930.63.3.185]
[PMID: 9289813]
[PMID: 17362465] [DOI: 10.1111/j.1442-9071.2006.01439.x]
[PMID: 21804938] [PMCID: 3144671] [DOI: 10.1155/2011/743597]
[PMID: 18658112] [DOI: 10.1164/rccm.200805-670OC]
[PMID: 20507930] [PMCID: 7965483] [DOI: 10.3174/ajnr.A2158]
[PMID: 17488505] [PMCID: 1871602] [DOI: 10.1186/1742-6405-4-9]
[PMID: 19365271] [DOI: 10.1097/QAI.0b013e3181a56f2e]
[PMID: 10351953] [DOI: 10.1164/ajrccm.159.6.9807152]
[PMID: 10426909] [DOI: 10.1016/s0190-9622(99)70364-6]
[PMID: 12194745] [DOI: 10.1258/095646202760159747]
[PMID: 9546531] [DOI: 10.1016/S0140-6736(05)79022-X]
[PMID: 12715328] [DOI: 10.1086/368311]
[PMID: 11192862] [DOI: 10.1097/00002030-200101050-00026]
[PMID: 16325657] [DOI: 10.1016/j.semarthrit.2005.03.007]
[PMID: 19483618] [DOI: 10.1097/QCO.0b013e32832d7aff]
[PMID: 17366961] [DOI: 10.2519/jospt.2007.2312]
[PMID: 17511865] [PMCID: 1884162] [DOI: 10.1186/1752-1947-1-22]
[PMID: 20015057] [DOI: 10.1111/j.1468-3083.2009.03549.x]
[PMID: 16394302] [DOI: 10.1056/NEJMra050408]
[PMID: 22728033] [PMCID: 3538487] [DOI: 10.1016/j.mayocp.2012.06.003]
[PMID: 6862066]
[PMID: 1226935]