Main article: Forms and structure of vitamin D

Table of Contents
Science behind vitamin D
A number of studies have suggested that patients with chronic inflammatory diseases are deficient in 25-hydroxyvitamin D (25-DThe vitamin D metabolite widely (and erroneously) considered best indicator of vitamin D "deficiency." Inactivates the Vitamin D Nuclear Receptor. Produced by hydroxylation of vitamin D3 in the liver.) and that consuming greater quantities of vitamin D, which further elevates 25-D levels, alleviates disease symptoms.
“Nowadays it is virtually impossible to buy milk in the US that has not been laced (‘fortified’) with vitamin D. The amounts added, and the content, have been subject to dubious control, and a number of fatalities have occurred due to Vitamin D poisoning from milk.”
“The mis-labeling of this compound as a vitamin is regrettable, as it gave a potential toxin an aura of undeserved innocence. Vitamin D is not a vitamin, but a steroid, which is, in its most active form, a powerful hormone with receptors widely distributed in the tissues of the body. As with other steroids, excessive consumption has risks.” Dr Hywel Davies
Some years ago, molecular biology identified 25-D as a secosteroid. Secosteroids would typically be expected to depress inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue., which is in line with the reports of short-term symptomatic improvement. The simplistic first-order mass-action model used to guide the early vitamin studies is now giving way to a more complex description of action.
When active, the Vitamin D nuclear receptorA nuclear receptor located throughout the body that plays a key role in the innate immune response. (VDRThe Vitamin D Receptor. A nuclear receptor located throughout the body that plays a key role in the innate immune response.) affects transcription of at least 913 genes and impacts processes ranging from calcium metabolism to expression of key antimicrobial peptidesBody’s naturally produced broad-spectrum antibacterials which target pathogens.. Additionally, recent research on the Human MicrobiomeThe bacterial community in the human body. Many species in the microbiota contribute to the development of chronic disease. shows that bacteria are far more pervasive than previously thought, dramatically increasing the possibility that the spectrum of chronic diseases is bacterial in origin.
Emerging molecular evidence suggests that symptomatic improvements among those administered vitamin D is the result of 25-D’s ability to temper bacterial-induced inflammation by slowing VDR activity. While this results in short-term palliation, persistent pathogens that influence disease progression proliferate over the long-term.
Forms and structure of vitamin D
All forms of vitamin D are secosteroids, sharing a close structural and functional resemblance to steroids. The full implications of a “vitamin” acting as a steroid has yet to be fully appreciated by many in the research community. The overlap between steroids and secosteroids is key to understanding the Marshall Pathogenesis. It explains how this “vitamin” can exert short-term palliative effects and long-term harm. Patients on the MP are advised to avoid consuming vitamin D, because of its immunomodulatory effects.
Steps for synthesis of vitamin D
There are a number of vitamin D metabolites in the body. The steps by which one form of vitamin D changes into the next are as follows:
- The body has natural stores of 7-dehydrocholesterolA cholesterol precursor manufactured by humans. When exposed to ultraviolet light converted into vitamin D3. Also known as previtamin-D3., a cholesterol precursor.
- When exposed to energy, specifically ultraviolet light, 7-dehydrocholesterol becomes pre-vitamin D3Largely inactive vitamin D metabolite naturally occurring in the human body. When exposed to ultraviolet radiation converted into 25-D. Also known as 7-dehydrocholesterol.
- Pre-vitamin D3 spontaneously isomerizes to Vitamin D3Form of vitamin D made in the skin when exposed to light. Also available in fish and meat. This secosteroid is sometimes converted into 25-D. Also known as cholecalciferol and activated 7-dehydrocholesterol. via a process called sigmatropic shift.
- In addition to the endogenous production of Vitamin D3, people get D3 from animal meats. Vitamin D2Form of vitamin D created by plants and fungi. When ingested the secosteroid is (sometimes) converted into 25-D. Also known as ergocholecalciferol. is found in plants and fungi, and is functionally similar to D3.
- Vitamin D3 and D2 are hydroxylated in the liver, and becomes 25-hydroxyvitamin D (25-D).
- 25-D is further hydroxylated by the enzyme 1α-hydroxylase, into the main biologically active hormone 1,25-dihydroxyvitamin DPrimary biologically active vitamin D hormone. Activates the vitamin D nuclear receptor. Produced by hydroxylation of 25-D. Also known as 1,25-dihydroxycholecalciferol, 1,25-hydroxyvitamin D and calcitirol. (1,25-DPrimary biologically active vitamin D hormone. Activates the vitamin D nuclear receptor. Produced by hydroxylation of 25-D. Also known as 1,25-dihydroxycholecalciferol, 1,25-hydroxyvitamin D and calcitirol.). While this reaction was originally thought to occur only in the kidneys, is now known to take place in tissues throughout the body, including within white blood cells called macrophages.
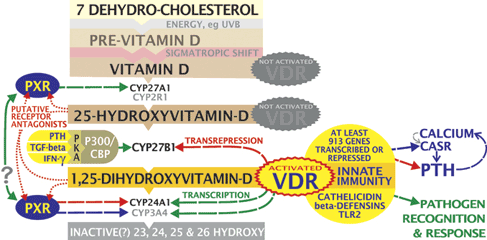
It's important to understand that the body tightly regulates the different forms as it might a steroid.
Metabolism of vitamin D and the Vitamin D Receptor in chronic disease
Main article: Metabolism of vitamin D and the Vitamin D Receptor
Supplemental vitamin D tends to be immunosuppressive
Related section: Sunlight can be immunosuppressive
Supplemental vitamin D has been widely lauded for conferring immunosuppressive effects.
Vitamin D affects the immune system at many levels and by a number of mechanisms…. Vitamin D has multiple immunosuppressant properties…. On the whole, vitamin D confers an immunosuppressive effect.
Aronson, Amital, and Shoenfeld 2)
Supplemental vitamin D is being touted as having a wide range of benefits in different diseases. A puzzling picture that emerges from the totality of the diseases that they are claimed to affect beneficially, is the belief that supplemental vitamin D will both reduce infections and suppress the immune system at the same time. While it is clear that there exist substances that can be “immunomodulating”, implicating that it can increase production/release of both immunosuppressive and immune activating substances, the important question is what the overall effect is. It is hard to envision that a substance can have strong anti-infectious properties while at the same time having a strong immune suppressive effect.
Supplemental vitamin D show no consistent effects on infection
In studies on acute respiratory tract infection3), tuberculosis4) and overall infections5), the effects of vitamin D have been mixed (and largely unsuccessful) in terms of reducing infectious burden.
A complete evaluation of the above mentioned studies, and the differences between them that can help explain the different results, is not suited for this article. However, on a general basis, one of the reasons for differing effects may be that vitamin D works differently in relatively healthy people as compared to sick people. Thus, vitamin D supplementation may give a marginal benefit in preventing infections in healthy people (see section below), but not in sick people. As of today (Dec 2012) we are not aware of any studies that have shown an actual reduction in infections in sick people (for instance tuberculosis or COPD) by vitamin D supplementation, as measured by culture or genetical detection methods. Furthermore, a general trend seems to be that apparent beneficial effects on infection in healthy people are not seen in individuals who have 25-hydroxyvitamin D levels within the normal range6)7)8), adding, as a side point, further weight to the mega dose vitamin D supplementation craze being without merit.
It is however not certain, in spite of some reported benefits in a few studies, that any level of supplementation is beneficial in terms of reducing infection. The studies are still too few to draw firm conclusions, and publication bias, as in any field science, may skew the overall results. Another factor which makes the reported benefits doubtful is that not all studies have reported an actual reduction in infection, but merely symptom based outcomes. Symptom based outcomes are relevant, but in light of the symptom reducing effects therapies that are immune suppressive may have, it is not clear that symptom reduction in the vitamin D supplementation studies are due to an actual reduction in infection. Further, most of the symptoms in upper respiratory tract infections are caused by the body's own immune response, and not the infectious agents9).
In sick people vitamin D supplementation increases infectious burden, and suppresses the immune system:
- monocytes – According to a 2011 interventional study in which patients with multiple sclerosis were given high doses of vitamin , peripheral blood mononuclear cells (monocytes) lose “abnormal reactivity” at 40 ng/mL.10)
- Epstein Barr virus – In a 2010 study of pregnancy-associated breast cancer, higher levels of 25-D were positively correlated with serum antibodies to Epstein Barr Virus, suggesting that EBV is able to better proliferate in patients who take vitamin D.11)
- toll-like receptors – As discussed elsewhere, the toll-like receptors (TLR) represent an ancient front-line defense system that enables the host organism to sense the presence of microbial components within minutes. As inducers of inflammation, TLRs act as important triggers of distinct entities such as sepsis or autoimmune disease exacerbation.12) For example, found that the TLRs are naturally upregulated in the autoimmune disease, Behcet's disease.13) However, a 2006 study showed that vitamin D3 suppresses the expression of TLR2A receptor which is expressed on the surface of certain cells and recognizes native or foreign substances and passes on appropriate signals to the cell and/or the nervous system. and TLR4 protein and mRNA in human monocytes in a time- and dose-dependent fashion.14) Dickie et al. further showed that expression of TLR9 was downregulated in monocytes by vitamin D3 supplementation.15)
- reduction in levels of inflammation – A 2011 study showed that in colorectal adenoma patients, the vitamin D supplementation group, TNF-alphaA cytokine critical for effective immune surveillance and is required for proper proliferation and function of immune cells. decreased 13%, IL-6 32%, IL-1 beta 50%, and IL-8 15% relative to placebo.16)
- short-term symptom resolution – Further evidence for vitamin D’s activity as an immunosuppressant comes in the range of reports of short-term symptom resolution in autoimmuneA condition or disease thought to arise from an overactive immune response of the body against substances and tissues normally present in the body patients taking vitamin D. Online forums are full of such reports.
Role in select diseases and conditions
The following articles discuss the role of vitamin D in select diseases. A more complete list of diseases that have been shown to have low level of 25-D is also available.
Osteoporosis
Main article: Osteoporosis and osteopenia
Related article: Secondary hyperparathyroidism
Both osteoporosis and osteopenia are diseases marked by a decrease in bone mineral density. Osteopenia is a less severe form of and sometimes precursor to osteoporosis. The loss of bone mass leads to a porous bone structure, frequent fractures, and delayed healing.
Among doctors, and even many researchers, it is conventional wisdom that vitamin D supplementation reverses osteopenia and osteoporosis. However, a growing body of interventional trials and molecular evidence shows this is not the case.
Thumbs Down on Calcium and Vitamin D to Prevent Hip Fracture January 2018
Supplementation and Fracture Incidence in Community-Dwelling Older Adults: A Systematic Review and Meta-analysis December 2017
Vitamin D Supplements Don't Help Bone Health, Meta-Study Finds October 2018
Instead, current research has demonstrated that osteoporosis and osteopenia are often the direct result of infection with the Th1 pathogens, a metagenomic microbiotaThe community of bacterial pathogens including those in an intracellular and biofilm state which cause chronic disease., which produce inflammatory cytokines and inactivate the Vitamin D Receptor. It seems the only way to achieve long-term reversal of bone loss is to kill the Th1 pathogens driving the disease process.
Rickets
Main article: Rickets (osteomalacia)
Rickets (osteomalacia) is a softening of the bones that leads to fractures and deformity. The majority of cases of rickets occur among children in developing countries who suffer from severe malnutrition. The disease is cited as a primary reason for consuming vitamin D regularly even though research has demonstrated that rickets is not caused by vitamin D deficiency but by hypophosphatemia.
The latest molecular evidence does not support adding high levels of vitamin D to the food chain in the name of “preventing rickets.” The health of the public would be much better served by regulations ensuring that they obtain adequate calcium and phosphorous rather than vitamin D.
Cancer
Main article: Vitamin D and cancer
A variety of studies have suggested that vitamin D protects against cancer. This seemingly intuitive proposition is supported by neither epidemiological nor molecular evidence. In fact, the very opposite is true. This article reviews why this body of research is most likely incorrect – or at the very least, much more complicated than articles in the popular media would have a person believe.
- Latitude studies - The “latitude studies” are observational, as opposed to interventional, studies, which use ambient solar UV radiation as a proxy for latitude and vitamin D status. For these studies, researchers compare rates of certain major cancers - most notably breast, colorectal and prostate cancer - to rates of sunlight exposure. This group of research has the liability of being wildly inconsistent. The choice to publish research on a specific latitude gradient may be a better proxy for a researcher's bias.
- Interventional studies - While some randomized controlled trials have suggested that consuming vitamin D reduces rates of cancer, larger and more carefully controlled studies show no such effect.
- Studies of vitamin D status - Many of the studies examining the relationship between vitamin D status and incidence of cancer argue that low levels of 25-D contribute to cancer. This conclusion has been invalidated by larger well-controlled studies. Although the immune system works to downregulate 25-D (25-hydroxyvitamin D) in inflammatory diseases such as cancer, very high levels of 25-D are a clear indication of regular supplementation. Studies suggest that consuming large amounts of vitamin D predispose a person to increased incidence of cancer.
- Observational studies – Some case control studies have found that vitamin D intake seems to increase incidence of certain types of cancer.
According to the Marshall Pathogenesis, alteration of vitamin D metabolism by a pathogenic microbiota prevents any benefit from vitamin D supplementation.
Cardiovascular disease
Main article: Cardiovascular disease
According to a 2010 paper by Swales and Wang, “despite substantial clinical evidence linking vitamin D deficiency with increased cardiovascular risk, it remains to be established whether this represents a causal association.”17) Indeed, data from a 2011 prospective, randomized, placebo-controlled trial[cite needed]18) has cast real doubt on the alleged cardioprotective benefits of vitamin D. Researchers performing a small study report that treatment with vitamin D for four months had no significant effect on endothelial function, vascular stiffness, or inflammation in healthy postmenopausal women.
A recent cross-sectional study involving 340 African Americans with type 2 diabetes found that serum 25-hydroxyvitamin D levels were positively associated with increased calcified atherosclerotic plaque in the aorta and carotid arteries.19)
Depression and seasonal affective disorder
Main article: Sunshine or light exposure as a therapy
Related articles: Latitude studies, Palliative vs. curative treatments
According to the Marshall Pathogenesis, light-related changes in mood can be attributed to fluctuations in 1,25-dihydroxyvitamin D (1,25-D). Such reactions exist in people who suffer from “seasonal affective disorder” as well as those who are addicted to or dependent upon tanning.
Contrary to popular belief, epidemiological research points to an increase in suicide across countries during the beginning of the summer months when people tend to get more light exposure.
Light exposure does nothing to resolve underlying disease state and can actually delay progress for Marshall Protocol (MP) patients. Certainly prolonged light exposure has been shown to increase skin melanoma – the World Health Organization now categorizes tanning beds under the highest cancer risk category.20)
MP patients who have completed the treatment have been able to attest to the fact that sunshine is not necessary for good health or happiness.
Despite what some researchers have argued, latitude studies that try to tie ambient solar UV radiation to prevalence of disease have been inconclusive.
Bioavailability
Impact of 25-hydroxyvitamin D, free and bioavailable fractions of vitamin D, and vitamin D binding protein levels on metabolic syndrome components 21)
Pregnancy
Main article: Pregnancy and vitamin D
Related article: Pregnancy and fertility
1,25-D rises by 40% in the early pregnant decidua, meaning that its ability to dysregulate the nuclear receptors and the antimicrobial peptides (AmPs) they express is particularly prevalent during the first trimesters of pregnancy. The subsequent decrease in immune function slows immunopathology, resulting in symptomatic relief. But when the surge in 1,25-D disappears after pregnancy, AmP expression and immunopathology increase once again, leading to exacerbation of disease symptoms. This may explain why some women with autoimmune disease experience periods of palliation during gestation only to become increasingly symptomatic after giving birth.
Problems with some vitamin D research
Insufficient followup of study subjects
Related articles: Innate immunity, About Radio Frequency Radiation
One of the abiding weaknesses of studies on the effects of vitamin D on health is that researchers simply do not follow subjects consuming the secosteroid for a sufficient period of time. Instead, they tend to track subjects over the course of weeks, months, or one or two years, during the period of time when study participants are usually feeling the palliative effects of the steroid.
This practice is a mistake as it does not account for the long-term immunosuppressive effects of a steroid. For example, the U-shaped relationship between vitamin D levels and long-term outcome in large cohort 22)
Failing to control for biases inherent to observational studies
Main article: Bias in observational epidemiological studies, Latitude studies
It is arguably impossible to sufficiently control for the socioeconomic factors, which drive a person to participate in a therapy or take a supplement. The case of hormone replacement therapy (HRT) is instructive. For decades, researchers thought that HRT prevented disease, but it was ultimately shown that it caused it.
Studies of vitamin D's efficacy are especially fraught with challenges. For one, the secosteroid is palliative and the negative side effects can only be seen after decades of use. Also, people who take vitamin D are demonstrably different than those who don't. They almost always have a higher socioeconomic status.
Not all studies on vitamin D's efficacy are observational, but those that are may warrant a special amount of skepticism.
Mistaking correlation for causation
Main article: Mistaking correlation for causation in vitamin D studies
Related article: Diseases associated with low levels of 25-D
Many vitamin D studies suffer from methodological errors including bias inherent to using self-selected subjects and insufficient followup, but perhaps their most egregious liability comes in mistaking correlation for causation. 23)
It's undisputed that a wide array of studies point to the fact that 25-hydroxyvitamin D (25-D) – typically referred to in the media as vitamin D – is low in people with numerous chronic inflammatory diseases. However, these studies fail to prove that low 25-D causes disease. Even so, some studies assume that doubling serum levels of 25-D would drastically reduce mortality.24)
In fact, molecular science has revealed that the levels of the vitamin D metabolites through a series of intricate and carefully controlled feedback pathways, mechanisms that belie the simplistic first-order mass-action model used to guide the short-sighted vitamin studies. Also, epidemiological evidence suggests that while 25-D is low in chronic disease, 1,25-D (1,25-dihydroxyvitamin D) tends to be very high, an observation which is at odds with the theory that vitamin D deficiency causes or exacerbates disease.
There have been lots of observational studied showing an association between various diseases and vitamin D deficiency, but there is not any evidence yet that that is a casual relationship… it may be that vitamin D deficiency is a marker of ill health.
Dr. Ruth McQuillan, University of Edinburgh
Populations that avoid vitamin D remain healthy despite low levels of 25-D
According to Professor Roger Bouillon of the University of Leuven, “over one billion” people worldwide need to increase their vitamin D intake due to vitamin D “deficiency.”25) One Saudi study concluded that 87.8% of healthy men were “deficient.”
Yet, observational studies show that populations which avoid vitamin D consumption have naturally low levels of 25-D and remain healthy with such levels.
- healthy Chilean women – A study which tested the level of 25-D in 90 “healthy, ambulatory Chilean women” showed that 27% of the premenopausal and 60% of the postmenopausal women had 25-D levels under 20 ng/ml.26)
- healthy Saudi medical students – A 2012 study collected data from 95 male and 103 female students with an average age of 19.5 years old. In 100% of the students, the vitamin D level was considered low. The mean 25-D level was 26.83 nmol/L in males and 16.03 nmol/L in females.
- healthy Chinese infants – In a 1992 study, healthy full-term infants from China had serum concentrations of 25-D ranging from an average of 5 ng/ml to 14 ng/ml.29)
- healthy Omani women – A 2011 study of 41 apparently healthy women (ages 18-45 years) working at the Royal Hospital, Muscat, Oman found that all study subjects had 25-D levels below 50 nmol/L.30)
- young healthy adults in western India – Among young healthy adults from the western part of India, the average serum level of 25-D indicated vitamin D “deficiency”: 17.4 ng/ml.31)
- healthy Saudi Arabians – Severe hypovitaminosis D is widespread and more common in non-diabetics than diabetics in Saudi adults.32) Nevertheless, this 2010 study's authors conclude a bit bizarrely, “The study further underscores the need for vitamin D fortification of the Saudi diet, and the promotion of vitamin D supplementation in both groups.”
- healthy lactating mothers – Even when lactating mothers take all but exceedingly high levels of vitamin D – 6,000 IU which is 15 times the United States' Recommended Daily Intake – the vitamin D content in breast milk remains very low.33) This is confusing for advocates of vitamin D supplementation who would think that breastfeeding mothers would give their infant extra levels of vitamin D during formative stages of growth.
The Vitamin D Council, an organization that advocates vitamin D supplementation, stated:
One of the great mysteries in human biology is the fact that most human breast milk is deficient in vitamin D. How could Nature overlook such an important nutrient in the “perfect food”?
Vitamin D Council
One research team, studying patients with xeroderma pigmentosum, a genetic disorder in which patients are unable to repair damage caused by ultraviolet light, found that vitamin D levels are maintained even when patients practice at least six years of rigorous photoprotection and not supplementing with vitamin D. More importantly, the researchers also concluded that the clinical manifestations of vitamin D “deficiency” were absent.
The patients all wore protective clothing and sunscreens when outdoors. Estimated mean vitamin D intake was normal. The mean values of serum 25-OHD were low normal, but 1,25-(OH)2D, calcium, ionized calcium and parathyroid hormone levels were normal [italics added]…. Despite rigorous sun protection normal vitamin D levels can be maintained in ambulatory patients with XP.
Armando Sallitto et al.34)
Ramifications of a simplistic understanding of vitamin D metabolism
Numerous studies have identified patient populations that are “deficient” in vitamin D. Patients suffering from obesity, schizophrenia, fibromyalgia, multiple sclerosis, autism, etc. all seem to be suffering from vitamin D deficiency. One could list hundreds of such studies.
Although it is not unheard of, few seem to explore the possibility that a low 25-D is the result of disease. Perhaps it is because researchers conceptualize vitamin D as they might a resource which gets used up and needs to be replenished – not unlike gasoline when a car runs low. This metaphor is not at all apt, because vitamin D is regulated like the steroid it is.35) 36)
Large segments of the population are consuming vitamin D at historic levels. Like the first-line treatment for many autoimmune diagnoses, the corticosteroidA first-line treatment for a number of diseases. Corticosteroids work by slowing the innate immune response. This provides some patients with temporary symptom palliation but exacerbates the disease over the long-term by allowing chronic pathogens to proliferate. Prednisone, vitamin D temporarily reduces symptoms of disease, but long-term use dramatically increases the odds of disease relapse.37)
In practice, widespread and systematic supplementation of vitamin D may serve to drive a kind of self-fulfilling prophesy. When whole populations are given large amounts of vitamin D, the only members of that population who remain “deficient” are those whose immune systems are fighting disease by actively downregulating 25-D. In other words, the more rigorously vitamin D is added to milk, juice, snack bars, and breakfast cereals, the less likely it is that someone has low levels of vitamin D but no chronic disease.
Supplemental vitamin D given to healthy people
According to the Marshall Pathogenesis, limited amounts of vitamin D may be helpful for a time to healthy people. Because the body is able to properly regulate the VDR, ingested vitamin D is rapidly converted into 1,25-D, which activates the VDR. This may explain the one (barely) significant finding from a 2011 Cochrane systematic review.38) (Publication bias may have also tilted the findings towards intervention.) However, this is certainly no basis for forced fortification.
Marshall Protocol and vitamin D
As opposed to certain treatments which employ sunshine or light therapy, patients on the Marshall ProtocolA curative medical treatment for chronic inflammatory disease. Based on the Marshall Pathogenesis. (MP) use the VDR agonistA substance such as olmesartan (Benicar) or 1,25-D which activates the Vitamin D Receptor and transcribes the genes necessary for a proper innate immune response., olmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. , and pulsed, low-dose antibiotics to gradually eliminate the Th1 pathogensThe community of bacterial pathogens which cause chronic inflammatory disease - one which almost certainly includes multiple species and bacterial forms.. Patients on the treatment must refrain from supplementing with vitamin D or eating any foods that contain vitamin D. These measures allow 25-D levels to drop to a point where the VDR can most optimally activate the innate immune system.
Because the vitamin D metabolites are dysregulated in chronic disease, most patients on the MP also become sensitive to light. Although light sensitivity improves as the Th1 pathogens are killed, most patients must avoid bright sunlight and block bright light in the eyes with special sunglasses during the healing process. However, once the Th1 pathogens have been killed and the vitamin D metabolites have re-stabilized, patients are able to tolerate sunlight and bright lights once again.
Related publications and presentations
Learn more
- Second-guessing the consensus on vitamin D – a critical analysis of research used to support increasing population-wide levels of vitamin D supplementation
- Children born and living without sunlight – In 2012, it was learned that 27 children had been living underground as members of a Muslim sect. Many had lived there for their entire lives and had never seen daylight. The conditions of these children was pronounced as “satisfactory” by pediatricians.
- The Truth About Vitamin D – plain language summary of the evidence for vitamin D, as of 2011
[PMID: 20736230] [PMCID: 2945184] [DOI: 10.1101/gr.107920.110]
[PMID: 17557889] [PMCID: 1955167] [DOI: 10.1136/ard.2007.069831]
[PMID: 23220552] [DOI: 10.1016/j.jsbmb.2012.11.017]
[PMID: 19179490] [DOI: 10.1164/rccm.200804-567OC]
[PMID: 17702768] [DOI: 10.1093/ageing/afm091]
[PMID: 22250141] [DOI: 10.7326/0003-4819-156-2-201201170-00004]
[PMID: 23032549] [DOI: 10.1001/jama.2012.12505]
[PMID: 19296870] [DOI: 10.1017/S0950268809002404]
[PMID: 18658112] [DOI: 10.1164/rccm.200805-670OC]
[PMID: 21697250] [PMCID: 3417163] [DOI: 10.1210/jc.2011-0325]
[PMID: 20691583] [DOI: 10.1016/j.ejca.2010.07.006]
[PMID: 16402404] [DOI: 10.1002/eji.200425995]
[PMID: 18411217] [DOI: 10.1093/rheumatology/ken109]
[PMID: 20435648] [DOI: 10.1093/rheumatology/keq124]
[PMID: 21724580] [PMCID: 3188339] [DOI: 10.1158/1940-6207.CAPR-11-0105]
[PMID: 20616710] [DOI: 10.1097/HCO.0b013e32833cd491]
[PMID: 20061416] [PMCID: 2841532] [DOI: 10.1210/jc.2009-1797]
[PMID: 19655431] [DOI: 10.1016/s1470-2045(09)70213-x]
[PMID: 28721141] [PMCID: 5510509] [DOI: 10.5114/aoms.2016.58594]
[PMID: 27589046] [DOI: 10.1016/j.ijcard.2016.08.322]
[PMID: 27610068] [PMCID: 5003588]
[PMID: 21731036] [DOI: 10.1038/ejcn.2011.68]
[PMID: 17290161] [DOI: 10.1097/GME.0b013e31802c54c0]
[PMID: 16500882]
[PMID: 11840180] [DOI: 10.1038/sj.ejcn.1601284]
[PMID: 1578308] [DOI: 10.1016/s0022-3476(05)80236-7]
[PMID: 21509209] [PMCID: 3074691]
[PMID: 21508424] [DOI: 10.1136/pgmj.2010.113092]
[PMID: 20635011]
[PMID: 17661565] [DOI: 10.1089/bfm.2006.1.59]
[PMID: 9418761] [DOI: 10.1016/s0190-9622(97)70069-0]
[PMID: 19444938] [DOI: 10.1016/j.jsbmb.2009.01.001]
[PMID: 18754003] [DOI: 10.1038/clpt.2008.165]
[PMID: 9118698] [DOI: 10.1378/chest.111.3.623]
[PMID: 21735411] [DOI: 10.1002/14651858.CD007470.pub2]
[PMID: 10919943] [DOI: 10.1093/ajcn/72.2.472]
[PMID: 19349547] [PMCID: 2674001] [DOI: 10.1200/JCO.2008.19.6162]
[PMID: 20016691] [PMCID: 2794851] [DOI: 10.1186/1710-1492-5-8]



