Main article: Statins and other anti-cholesterol drugs

Table of Contents
Tests: cholesterol and triglycerides (lipids)
The lipid profile is a group of tests that are often ordered together to determine risk of coronary heart disease such as heart attack or atherosclerosis. The lipid profile typically includes:
- high density lipoprotein cholesterol (HDL-C) — often called “good” cholesterol
- low density lipoprotein cholesterol (LDL-C) — often called “bad” cholesterol
- total cholesterol
- triglycerides
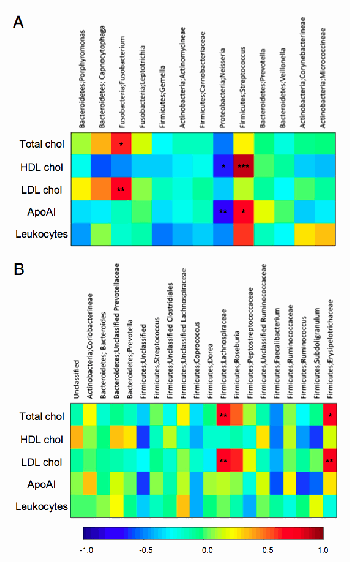
In many of the diseases the Marshall Protocol (MP) treats, patients may present with elevated cholesterol. Traditionally, it has been assumed that the elevated cholesterol is causing or contributing to the disease process. However, the alternate hypothesis is no less plausible; in certain inflammatory diseases, the body may be deliberately upregulating levels of cholesterol in order to better manage the disease process. Increasing evidence suggests that this alternative explanation may be true.1) 2) For example, a 2010 study found that several bacterial taxa in the oral cavity and the gut correlated with plasma cholesterol levels3), and another study found that high cholesterol protects against endotoxemia.4)
Both “good” and “bad” forms of cholesterol play pivotal roles in fighting infection, for example, scavenging endotoxins that are released during destruction of pathogenic bacterial forms. While higher levels of total cholesterol are associated with some forms of cardiovascular disease in some patient populations, a number of statistically significant inverse correlations have been found between total cholesterol and various diseases including chronic heart failure, respiratory and gastrointestinal diseases, and various acute infections.
Thus, high cholesterol levels among patients on the MP are not seen as a problem but as a sign of the inflammatory response to infection. This means that MP patients do not need to take any measures to lower cholesterol. Over time, as the MP medications work to gradually lower infectious agents causing inflammation, it is expected that cholesterol will return to a normal range. In this same vein, statins, in particular, should not be used to lower cholesterol, because they have effects on the same receptors as olmesartan, which may prevent the drug from working effectively.
<html><!– Most researchers today consider that a high intake of saturated fat and elevated LDL cholesterol are the most important causes of atherosclerosis and coronary heart disease. This lipid hypothesis has dominated cardiovascular research and prevention for almost half a century although the number of contradictory studies may exceed those that are supportive.5)
Both “good” and “bad” form of cholesterol play pivotal roles in fighting infection, for example, scavenging endotoxins that are released during destruction of pathogenic bacterial forms. While higher levels of total cholesterol are associated with some forms of cardiovascular disease in some patient populations, a number of statistically significant inverse correlations have been found between total cholesterol and various diseases including chronic heart failure, respiratory and gastrointestinal diseases, and various chronic infections as well.
There is also broad evidence that cholesterol does not promote plaque as evidenced by studies that show therapies which directly lower cholesterol may make patients sicker. The article devoted to statins reviews the evidence that statins offer mild protection against disease not through its effect on cholesterol but through their underreported immunomodulatory properties.
Some patients on the Marshall Protocol (MP) have reported temporary increases in cholesterol and triglycerides, an observation which is consistent with a heightened immune response.
–></html>
Statins and other anti-cholesterol drugs
Related articles: Tests: cholesterol and triglycerides (lipids), Palliative vs. curative treatments
The statins (or HMG-CoA reductase inhibitors) along with other drugs, such as cholestyramine (Questran), comprise the class of hypolipidemic drugs. Hypolipidemic drugs are prescribed - sometimes aggressively so - to lower cholesterol levels in people with or at risk of cardiovascular disease and certain inflammatory diseases such as sarcoidosis. Statins are prescribed even though their full mechanisms of action remain unclear. One strong possibility is that statins exert their effects via the body's nuclear receptorsIntracellular receptor proteins that bind to hydrophobic signal molecules (such as steroid and thyroid hormones) or intracellular metabolites and are thus activated to bind to specific DNA sequences which affect transcription., which are intricately connected to innate immune function.
The statins have a range of documented negative effects, some of which may be immunopathological. Because statins may interfere with the Marshall ProtocolA curative medical treatment for chronic inflammatory disease. Based on the Marshall Pathogenesis., these drugs are contraindicated.
Statins interfere with the actions of OlmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. , as they are a very similar molecule, and compete with Olmesartan for many of Olmesartan's molecular binding sites. The actions of statins on the Nuclear Receptors are therefore competitive with Olmesartan, as they reduce or negate Olmesartan's therapeutic activities.
As the 2008 ENHANCE trial illustrates, while high cholesterol is correlated with increased incidence of diseases, lowering cholesterol does not appear to improve human health.6) Indeed, there is some evidence this type of intervention does the opposite.7)
Cholesterol contributes to a robust immune response
While there's no doubt plasma lipoproteins function primarily in shuttling lipids among tissues and organs:
Cumulative evidence suggests that lipoproteins may also prevent bacterial, viral and parasitic infections and are therefore a component of innate immunity. Lipoproteins can also detoxify lipopolysaccharide and lipoteichoic acid. Infections can induce oxidation of LDL, and oxLDL in turn plays important anti-infective roles and protects against endotoxin-induced tissue damage. There is also evidence that apo(a) is protective against pathogens. Taken together, the evidence suggests that it might be valuable to introduce the concept that plasma lipoproteins belong in the realm of host immune response.
R. Han 8)
Laboratory evidence
Several researchers have suggested that the blood lipids play a pivotal role in the immune defense system.9) 10)
- High total cholesterol is correlated with markers of immune function – Men with low cholesterol had significantly fewer circulating lymphocytes, total T cells, helper cells, and CD8+ cells than men with high cholesterol.11) Also, adhesiveness to plastic surface, phagocytic activity and spontaneous motility of mononuclear cells from hypercholesterolaemic individuals were significantly higher compared to controls.12)
- Bacterial endotoxins are bound by cholesterol – Lipoproteins play important roles in the process of removing toxic bacterial cell wall constituents including peptidoglycans and lipoteichoic acid, and lipopolysaccharide (endotoxins), all of which can contribute to bacterial sepsis and septic shock.13) In addition, lipopoteins scavenge the main pathogenic component of the cell walls of Gram-negative bacteria; endotoxins (which are released during immunopathology) are rapidly bound by LDL cholesterol.14) 15) Another example: Staphylococcus aureus-toxin, a toxin produced by most pathogenic Staphylococcus strains and causing damage to a wide variety of cells, is bound and almost totally inactivated by human serum and purified LDL.16)
Epidemiological and clinical evidence
Many epidemiological and clinical observations are in accord with the laboratory studies.17) Statistically significant inverse correlations have been found between total cholesterol and various diseases (i.e. higher cholesterol is correlated with lower disease incidence):
- pneumonia, influenza, and other infectious diseases – In a 15 year follow-up study of more than 120,000 individuals, Iribarren et al. found a strong inverse association between total cholesterol (as determined initially) and the risk of being admitted to hospital due to an infectious disease.18) In a similar study of more than 100,000 individuals followed for 15 years, a strong, inverse association was found between total cholesterol and the risk of being admitted to hospital because of pneumonia or influenza.19) Individuals with familiar hypercholesterolaemia had a longer life expectancy than others before year 1900, where the main cause of mortality was infectious diseases.20)
- HIV/AIDS – In a study of 2,446 unmarried men with a previous history of sexually transmitted disease or liver disease followed for 14 years, a multivariate-adjusted analysis showed a risk ratio for HIV infection of 1.66 (95%CI 1.07–2.56) in the lowest cholesterol quartile compared with the risk in the second quartile.21) In accordance, an inverse association between total cholesterol and the risk of death in AIDS was found in a follow-up of AIDS patients.22)
- various other infections – Statistically significant, inverse associations were found for urinary tract infections, all genitourinary infections and miscellaneous viral infections for women, and for urinary tract infections, musculo-skeletal infections and skin and subcutaneous infections in men.23) Low total cholesterol predicts mortality in patients with postoperative abdominal infections.24))
Higher levels of cholesterol are also associated with lower prevalence of disease in systems susceptible to infections including the respiratory system and the gastrointestinal tract. A meta-analysis of 19 cohort studies including 68,406 deaths, found an inverse correlation between total cholesterol and mortality from respiratory and gastrointestinal diseases.25)
Cholesterol may not cause cardiovascular disease
According to the widely accepted belief, high LDL cholesterol promotes the development of atherosclerosis, and, therefore, cardiovascular disease. However, there is a great deal of contradictory evidence.26) 27) 28)
- High total cholesterol is not associated with all cardiovascular diseases in all patient groups – If high total cholesterol or LDL cholesterol were the most important cause of cardiovascular disease, it should be a risk factor in both sexes, in all populations, and in all age groups, but it is not. In many populations – including women, Canadian and Russian men, Maoris, patients with diabetes, and patients with the nephrotic syndrome – the association between total cholesterol and mortality is absent or inverse.29) Similarly, the results of the Framingham study, one of the largest studies on cardiovascular disease conducted to date, found that for both men and women over 50 years of age, life expectancy showed no association with cholesterol levels. The likelihood of suffering a fatal first heart attack was no less for those with a cholesterol level of 180 mg/dl than it was for those with 250. In fact, those Framingham residents whose cholesterol declined over the first 14 years of observation were more likely to die prematurely than those whose cholesterol remained the same or increased.30)
- High levels of HDL (“good”) cholesterol do not predict coronary heart disease or all-cause mortality – This lack of an effect is especially apparent in old people.33) Notably, the greatest prevalence of cardiovascular disease are seen in older people.
- Statins' effect on cardiovascular diseases may be independent of their ability to lower cholesterol34) – A seminal study called the ENHANCE trial was published in 2008. The trial tested the effects of a new cholesterol-lowering medication called Zetia (which works by decreasing cholesterol absorption in the intestine) on patients with cardiovascular disease. It found that Vytorin, a combination pill containing both Zetia and the statin Zocor (simvastatin), proved better than the statin alone at reducing levels of cholesterol. However, ENHANCE collaborators reported that Vytorin resulted in growth of plaque.35) For these reasons, several researchers have proposed that statins have an entirely different primary mode of action.
Atherosclerosis
- Some angiographic studies show that cholesterol is inversely associated with atherosclerosis – In two of five angiographic (x-rays of blood vessels) studies, there was an inverse association between change of total cholesterol and atherosclerotic growth.36)
- Diets intended to lower cholesterol do not lead to reduced atherosclerosis – In 2006, the Cochrane Collaboration published an update of a systematic review that analyzed 10 of the most rigorous studies to test the ability of “multiple risk factor interventions” (i.e. diets in low saturated fat, smoking cessation, etc.) to prevent cardiovascular disease. Together the trials accounted for around 900,000 patients, many of which were followed over the course of several years. The analysis found that interventions designed to lower risk factors for cardiovascular disease such as diet counseling were ineffective: “The pooled effects suggest multiple risk factor intervention has no effect on mortality…. The evidence suggests that such interventions have limited utility in the general population.”37) In the only clinical trial of the effect of diets high in unsaturated fats on atherosclerosis that included a post-mortem, complicated atherosclerosis was most pronounced in the treatment group.38)
Stroke
- Stroke mortality is not associated with cholesterol – A 2007 Lancet meta-analysis of 61 prospective observational studies, representing 900,000 patients, found that there was no independent positive association of cholesterol with stroke mortality, especially at older ages or higher blood pressures.39)
Heart attack
- Heart attack mortality is not associated with cholesterol – The World Health Organization's MONICA Project, begun in the 1970s, has been described as “far and away the biggest international collaborative study of cardiovascular disease ever carried out.” By the late 1990s, MONICA had recorded 150,000 heart attacks and analyzed 180,000 risk factor records. Heart disease mortality was declining worldwide but that decline was independent of cholesterol levels, blood pressure, or even smoking habits.40)
Chronic heart failure
- Low total cholesterol is correlated with worse outcomes in chronic heart failure – In patients with oedematous chronic heart failure, low total cholesterol predicts impaired perioperative and long-term survival. As such patients show substantial immune activation and have raised plasma concentrations of bacterial lipopolysaccharide, Rachhaus et al. have suggested that high total cholesterol has a protective effect in such patients.41) Several commentators have further argued that cholesterol's ability to scavenge endotoxins explains why patients with higher level of cholesterol do better:
The pathophysiologic understanding of chronic heart failure has made significant advances over the last decades. Counterintuitively, high levels of plasma cholesterol are associated with better survival, perhaps because plasma lipoproteins are able to scavenge lipopolysaccharide, a cell-wall component from gram-negative bacteria. A number of similar features are present in patients who have sepsis.
S. von Haehling et al.42)
There is some evidence that lower serum cholesterol concentrations (as a surrogate for the totality of lipoproteins) relate to impaired survival in patients with chronic heart failure (CHF). Inflammation is a feature in patients with CHF and increased lipopolysaccharide may contribute substantially. We postulate that higher concentrations of total cholesterol are beneficial in these patients. This is potentially attributable to the property of lipoproteins to bind lipopolysaccharide, thereby preventing its detrimental effects.
M. Rauchhaus et al.43)
Patients experiences
[My physician] remarked on my astounding cholesterol improvement in the last year (from 311 to 191 mg/dL, and my triglycerides are down from 129 to 68 since 1 year ago) and he explained that this could be from weight loss (no, weight has been stable except for slight recent gain since adding Bactrim) or change of diet (no), or exercise (no). I told him the only thing I've done differently is the MP. Cue the skeptical look.
MrsKeeper, MarshallProtocol.com
I got my blood work results today…. My triglyceride level went from 450 down to 125 without statins, change of diet or exercise…. I don't have problems with my heart rhythms any longer and having my count drop like that was pure joy.
Dolores P. Rosner (martysfolks), MarshallProtocol.com
I went to see my doctor yesterday and she told me the results of my blood tests were all normal so I am pleased about that. My cholesterol is normal and it looks like the MP has done the trick as I stopped taking statins almost a year ago.
Hester33, MarshallProtocol.com
[PMID: 14631060] [DOI: 10.1093/qjmed/hcg150]
[PMID: 20377753] [DOI: 10.1111/j.1348-0421.2010.00203.x]
[PMID: 20937873] [PMCID: 3063583] [DOI: 10.1073/pnas.1011383107]
[PMID: 21711511] [PMCID: 3146904] [DOI: 10.1186/1477-5956-9-34]
[PMID: 18615352] [DOI: 10.1080/14017430801983082]
[PMID: 18376000] [DOI: 10.1056/NEJMoa0800742]
[PMID: 9245545] [DOI: 10.1006/clin.1997.4382]
[PMID: 1631799] [DOI: 10.1016/0049-3848(92)90164-6]
[PMID: 12857774] [PMCID: 164216] [DOI: 10.1128/CMR.16.3.379-414.2003]
[PMID: 2114366] [PMCID: 258822] [DOI: 10.1128/iai.58.7.2375-2382.1990]
[PMID: 1547193] [DOI: 10.1161/01.atv.12.3.341]
[PMID: 6853557]
[PMID: 9825784] [PMCID: 2809530] [DOI: 10.1017/s0950268898001435]
[PMID: 9447398] [DOI: 10.1093/ije/26.6.1191]
[PMID: 1355411] [DOI: 10.1161/01.cir.86.3.1046]
[PMID: 9436759] [DOI: 10.1097/00042560-199801010-00008]
[PMID: 9189220]
[PMID: 8645072] [DOI: 10.1001/archsurg.1996.01430180067014]
[PMID: 9635993] [DOI: 10.1016/s0895-4356(98)00018-3]
[PMID: 12507667] [DOI: 10.1016/s0895-4356(02)00504-8]
[PMID: 2564950] [DOI: 10.1016/s0140-6736(89)92865-1]
[PMID: 9413489] [DOI: 10.1016/S0140-6736(05)63609-4]
[PMID: 12562541] [DOI: 10.1007/s11883-003-0067-1]
[PMID: 12037248] [DOI: 10.1093/qjmed/95.6.397]
[PMID: 17054138] [PMCID: 4160097] [DOI: 10.1002/14651858.CD001561.pub2]
[PMID: 18061058] [DOI: 10.1016/S0140-6736(07)61778-4]
[PMID: 10334252] [DOI: 10.1016/s0140-6736(99)04021-0]
[PMID: 11036910] [DOI: 10.1016/S0140-6736(00)02690-8]
[PMID: 18433694] [DOI: 10.1016/j.hfc.2008.01.009]

