Related article: Hypertension

Table of Contents
Low blood pressure and dizziness
Low blood pressure (hypotension) and dizziness are symptoms of Th1 diseaseAny of the chronic inflammatory diseases caused by bacterial pathogens. and can be exacerbated during recovery on the Marshall ProtocolA curative medical treatment for chronic inflammatory disease. Based on the Marshall Pathogenesis. (MP).
During bouts of hypotension, some physicians may be reluctant to continue prescribing olmesartan (Benicar)Medication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor., a medication which is otherwise used to reduce blood pressure. But, it is important that they do. OlmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. has an excellent safety profile and is only a weak hypotensive, reducing diastolic pressure by no more than 12 mm Hg in the dosages suggested by the Marshall Protocol guidelines.
Patients and their physicians are advised not to be overly concerned with symptoms of low blood pressure. They resolve as the disease does. Also, the symptoms thought to be due to low blood pressure have been shown to resolve even if the low blood pressure persists.
Concerns about "abnormally low" blood pressure
The NIH has created no medical standards that define low blood pressure, or a range in which low blood pressure is considered dangerous. In 2004, the NIH issued blood pressure guidelines for clinical practice. While three levels of hypertension are listed, these guidelines do not single out any range of blood pressures as being low or abnormally low – only blood pressures below 120/80 are considered to be normal.
We really don't consider blood pressure to be low unless the pressure will not support the person when (s)he goes from laying to sitting to standing. If (s)he can do that without blacking out, the pressure is fine.
Madwolf, PA, MarshallProtocol.com
Further, there is no proof that the values normally used to indicate low blood pressure in healthy patients have any relevance to Th1 inflammatory disease patients. Symptoms which appear to be caused by hypotension – dizziness, fatigue, lightheadedness – are a result of the disease and will resolve as the inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue. resolves no matter the number of the blood pressure.
Therefore, it is not necessary to monitor blood pressure while on the MP. Some MP physicians do not recommend blood pressure checks. They simply tell their patients to lie down if they feel dizzy. Even patients with extremely low blood pressure – 85/55 or lower – have been able to continue taking olmesartan (Benicar).
Concerns about the hypotensive effects of olmesartan
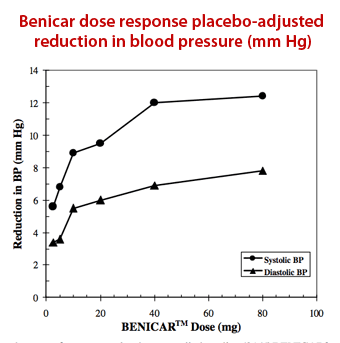
As it is otherwise used, the primary indication for olmesartan (Benicar) is as a mild hypotensive drug. As one can see from the FDA label for Benicar, the dose response curve for Benicar follows a horizontal parabola, with additional doses of the drug having incrementally smaller decreases in blood pressure. For example, the difference between 40mg and 80mg of olmesartan results in an increase of no more than 1mm Hg. This chart is for a single dose given at one time and does not account for a patient taking four doses over 24 hours nor does it show how doses of 160mg affect blood pressure. However, given the clarity of this trend, it is reasonable to assume that the additional effect on blood pressure of 160mg as compared to 80mg of olmesartan, at least when it comes to blood pressure, is limited.
It is important to understand that olmesartan’s effect on blood pressure is limited in order to appreciate that a decline in systolic pressure greater than 15mm Hg of mercury is not due to Benicar’s hypotensive action.
One such factor is the effect the widespread destruction of bacteria and human cells infected by bacteria can have on blood pressure. Though this isn’t true of all bacterial forms, when some forms of bacteria are destroyed, they release endotoxins,1) the bioavailability of which can lead to a steep decline in blood pressure.2) For example, one lab worker ingested very large amounts of salmonella endotoxin (much more than could ever be generated by an MP patient) and found his blood pressure drop to 42/20 mm Hg.3)
Safety profile of olmesartan
Main article: Safety of olmesartan (Benicar)
Olmesartan has an excellent safety profile.
When we visited the US FDA in Washington in April 2007, we were told that “Benicar is the safest drug in the US formulary.” I am at a loss to understand what the “side effects of Benicar” might be. I have been looking for them for six years, and all I can find is epidemic Th1 disease, and a consequent reaction to Benicar when patients' immune systems are activated to recognize the pathogens.
If blood pressure becomes too low, it is as a result of the disease, the immunopathology, as the drug doesn't have much pressor effect in healthy people (max 12 mm Hg).
Trevor Marshall, PhD
Blood pressure fluctations are due to the inflammatory disease not Benicar. Reducing the dose will eliminate the inflammatory blockade and make the situation worse.
Evidence of infectious cause
I believe chronic hypotension can be a side effect of a chronic endotoxemia Dmitry 2018
Endotoxemia causes hypotension characterized by vasodilation and resistance to vasopressor agents. 4)
…The resulting endotoxemia leads to systemic hypotension… 5)
see also
Interactions of Gut Microbiota, Endotoxemia, Immune Function, and Diet in Exertional Heatstroke
Elevated nitric oxide (NO) levels appear to be a primary cause of the sepsis related hypotension.
Nitric Oxide Measurements during Endotoxemia Brovkovych et al
Nitric oxide (NO), an endothelium-derived relaxing factor (EDRF), is released by different types of cells under the influence of endotoxin and various cytokinesAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. Is endotoxin-induced hypotension related to nitric oxide formation? Preiser et al
Endotoxemia causes hypotension characterized by vasodilation and resistance to vasopressor agents. 6)
Hypotension during endotoxemia in aged humans. 7)
Enhanced modulation of hypotension in endotoxemia by concomitant nitric oxide synthesis inhibition and nitric oxide scavenging. 8)
Symptom management
There are a number of generic strategies for managing immunopathology. The following measures particular to lightheadedness and dizziness may also be helpful:
- Patients should lie down as soon as they feel lightheaded or dizzy to keep from falling and hurting themselves if they do faint. If they're in a place where it's impossible to lie down, they should sit and try to put their head between your knees. Naturally, if they're doing anything that might put themselves or others at risk for injury, such as driving, they should stop right away. Lying on one's left side will maximize blood flow to the heart and thus to the brain. It will likely keep one from actually fainting and probably relieve the sensation of lightheadedness altogether.
- Learn the signs of lightheadedness. Feelings of warmth, paleness, sweating, and nausea as well as yawning, hyperventilation and straining to pee, cough or have a bowel movement can all precede lightheadedness.
- Do not stand up too fast. When suddenly standing up, blood pools in the feet and lower legs. This pooling can also happen as a result of prolonged standing. If one's body isn't able to adjust when standing, not enough blood returns to the heart from your legs and one's blood pressure drops quickly, which can leave a person feeling faint. When lying down, sit up slowly and stay sitting a few minutes with your legs dangling over the side of the bed. Then slowly rise from sitting to standing. If standing in one place for a long time, patients should move their legs to promote circulation.
- Wearing support stockings can help circulation in the lower half of the body.
- Strive to manage anxiety, a symptom which can sometimes make a person feel faint.
- Try not to get overheated. Spending time in a very hot room or taking a hot bath or shower can cause one's blood vessels to dilate, lowering your blood pressure and making one woozy. Avoid hot crowded places and wear clothing in layers so it can shed some as necessary. Take warm instead of hot showers or baths, and try to keep the bathroom cool.
- Eat adequate food and drink. Patients who don't eat enough can end up with low blood sugar, which can make them feel dizzy or faint. Dehydration and not eating enough salt can have a similar affect. Try to keep blood sugar from getting too low by eating small frequent meals during the day instead of three large ones. Carry healthy snacks whenever hungry.
Replacement of electrolytes
Related article: Test: Electrolytes
Typically, patients taking olmesartan do not have any problem with hyponatremia (low sodium). It would be incorrect to assume that one's sodium is low just because one's blood pressure is low. Concerned patients can ask their physician to test their sodium level.
Gatorade and other energy replacement drinks are not recommended. Even those which are low in sugar contain extra potassium which you may not need. However, these drinks may be helpful if a patient has chronic diarrhea or experiences a lengthy bout of severe diarrhea.
Symptoms associated with low blood pressure
Certain symptoms associated with low blood pressure – dizziness, vertigo, and fainting – are not caused by low blood pressure, but coincidental to it.
Dizziness
Many MP patients report symptoms of dizziness in the first week or weeks after taking olmesartan. This is due to initial hormonal fluctuations. For example, levels of 1,25-DPrimary biologically active vitamin D hormone. Activates the vitamin D nuclear receptor. Produced by hydroxylation of 25-D. Also known as 1,25-dihydroxycholecalciferol, 1,25-hydroxyvitamin D and calcitirol. sometimes fall by as much as 50% during this time.
Later on, during the treatment itself, low blood pressure is thought to be caused by the release of endotoxins during bacterial die-off, a necessary part of immunopathology. This totally upsets the body's hormonal balances. The readjustment process can cause symptoms such as vertigo and dizziness, which are from the disease – not from the lower blood pressure.
As the inflammation resolves with the MP, dizziness resolves also. The dizziness resolves even when the blood pressure remains low and the dosage of Benicar remains the same.
Vertigo
Vertigo, a type of dizziness, refers to the sensation of spinning or whirling that occurs as a result of a disturbance in balance (equilibrium). It also may be used to describe feelings of dizziness, lightheadedness, faintness, and unsteadiness. The sensation of movement is called subjective vertigo and the perception of movement in surrounding objects is called objective vertigo.
Vertigo usually occurs as a result of a disorder in the vestibular system – that is, structures of the inner ear, the vestibular nerve, brainstem, and cerebellum. The vestibular system is responsible for integrating sensory stimuli and movement and for keeping objects in visual focus as the body moves.
Vestibular rehabilitation therapy (VRT) is a type of physical therapy used to treat vertigo. In VRT, the patient performs exercises designed to allow the brain to adapt to and compensate for whatever is causing the vertigo.
Benign paroxysmal positional vertigo may be treated with meclizine (Antivert), an oral antiemetic that can be taken up to three times a day, or only as needed. Meclizine may cause drowsiness, dry mouth, and blurred vision.
Fainting
Fainting (syncope) is a transient loss of consciousness with an inability to remain upright that is followed by spontaneous recovery. The term syncope excludes seizures, coma, shock, or other states of altered consciousness. Cardiac causes should be ruled out when a syncopal episode occurs.
Fainting may be due to neurological immunopathologyA temporary exacerbation of neurological symptoms due to bacterial death. Requires careful management by physicians..
With regards to “fainting” episodes, it has been my observation of my own response and my patients that there are 2 different conditions. One is almost always postural and is benign. Being attentive to the possibility of fainting with change of position plus insuring adequate hydration and some salt intake is usually all that is necessary….
The other, in my opinion, is a mild seizure disorder due to neurological Herx reaction. This causes “blacking out” which does not require postural change, is usually associated with some form of aura, and causes a transient loss of consciousness. This, I believe, is due to glial cell apoptosis (die off) and subsequent transient dysruption of neuron function. If spells are frequent or severe, an anti-epileptic, such as gabapentin (Neurontin), may be necessary.
Besides myself, I have had several patients who have “blacked out.” These were not because of low blood pressure but were, I believe, a neurological event. It tends to occur in people with pre-existing neurological symptoms such as tinnitus, visual disturbance or paraesthesia. I found increasing hydration afterwards lessens after effects.
It also tends to become less frequent as one progresses and decreases the bacterial load. IMO, it is a Herx reaction affecting the electrical functioning of the brain, similar to the symptoms seen in the heart where conduction abnormalities are common in Th1 disease.
Greg Blaney, MD
It isn't necessary to force someone to wake up following fainting. Tell your family to make sure you are breathing and call for emergency assistance only if you do not arouse with normal stimulation of movement and noise, in a couple minutes.
Patients experiences
I checked my blood pressure for the first time for months the other day and was surprised to find it at 87/55, and I am not having dizzy spells as I was early in the Protocol when my blood pressure was low. I assumed my blood pressure was back to 120/80 or something considered more the norm. It was a pleasant surprise to find my blood pressure so low and my condition improving.
vda51, MarshallProtocol.com
When I started Benicar and became dizzy, I assumed it was my very low blood pressure. Trevor told me it was the disease causing the dizziness. I didn't believe him until months later when the dizziness had gradually subsided. I did notice once when I was hypovolemic that the dizziness was worse. But drinking enough fluids and getting enough salt in my diet is not a problem. I'm still taking Benicar every six hours and my blood pressure is usually 75/55 on a busy day. I experience very transient dizziness rarely now which I attribute to the immunopathology. Surely if it were my low blood pressure, I would be dizzy all the time.
My B/P in the middle of a busy workday is routinely 75/45. I have no symptoms related to this low blood pressure. I had some lightheadedness in the early days of the MP which gradually resolved as my inflammation resolved. I suspect that when Th1 inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue. is conquered, the medical community will have to redefine normal blood pressure.
Meg, MarshallProtocol.com
Taking less Benicar, as I know from experience, will only make you feel worse, but will not have any effect on the low numbers. One day, I took less, felt worse, and my BP was even lower than it was on the correct MP dosage! When my doctor realized that, she allowed me to take my Benicar as recommended, and with time, things settled down very well and she (and I) stopped worrying about low BP altogether. These day, four months into the MP, I still have some really low BP (around 75/45), but, ironically often feel much better then than I do at higher readings, which goes to prove that the Benicar is not causing your problem, but the disease process is. At my last doctor visit, I had a BP reading of 100/70, which is the highest I have ever been - even not on Benicar, and that day, I had taken it every 6 hours. Today, I am back to 76/46, and feel just fine there.
Even with my low BP, I have never passed out, I am able to lead a full life within the MP parmeters, and work as a teacher. I keep a bottle of water with me at all times, as the more hydrated I remain, the more stable my BP is, even if it is very low. If I feel bad during my working day, I take an extra 20 mg of Benicar, my BP goes up and I feel heaps better.
Kas, MarshallProtocol.com
Have been to have my kidney function and BP checked and everything is much improved! Having increased my Benicar frequency to 6-hourly my blood pressure has risen to a respectable 94/57. This is remarkable, as it had stabilized at 80/40 since I was in Phase 1. So this is a lesson to others whose doctors panic and say “Whoa, your BP is dropping, you should take less of that Benicar.” The counter-intuitive answer is to TAKE MORE instead.
Claudia, MarshallProtocol.com
[PMID: 7619330] [DOI: 10.2165/00002018-199512030-00004]
[PMID: 8479465] [DOI: 10.1056/NEJM199305203282005]
[PMID: 1602014] [PMCID: 295927] [DOI: 10.1172/JCI115820]
[PMID: 29850597] [PMCID: 5926483] [DOI: 10.1155/2018/5724575]
[PMID: 11553251] [DOI: 10.1046/j.1365-2346.2001.00958.x]
[PMID: 9083636] [DOI: 10.3109/10731199709118907]

