Presentation - Vitamin D metabolites as clinical markers in autoimmune and chronic illness
Type: Conference presentation
Presenter: Greg Blaney, MD
Conference: 6th International Congress on Autoimmunity
Location: Porto, Portugal
Date: September 11, 2008
Additional content: Notes from the 2008 International Congress on Autoimmunity by Amy Proal; PDF of transcript alongside slides
Transcript
Thank you for inviting me to come to this prestigious conference. I’m kind of a unique being because I’m a clinician, I’m not a researcher, I’m not an academic but I have been involved in clinical practice for too many years and the last 20+ has been dealing with chronic pain patients and (I’m a Mac guy so you have to give me a little pause cause I’m working with a PC…) …and in chronic pain patients -chronic pain manifesting most of the time in muscle-skeletal pain but also in neurological pain, discogenic pain etcetera- in that population of patients there is a number of co-morbid conditions. It is very common to find chronic fatigue syndrome(fibromyalgia), Irritable Bowel Syndrome, Interstitial cystitis, prostatitis, sinusitis, periodontal disease, osteoporosis, osteoarthritis, hypertension, renal calculi, colitisis and various cognitive and central nervous system disorders.
And they can be challenge. Now, in trying to find a way to support my patients in their chronic pain, there’s a fairly limited number of tools. In terms of fibromyalgia and muscle skeletal pain you know we have biomechanical factors, we have fitness factors, but other than that we are either working with muscle relaxants, NSAIDs, now we have got Neuronton, Lyrica but they have variable effectiveness and of course often have side effects and will actually aggravate some of co-morbid conditions. So in my kind of endeavors to try and discover what may be going on this with patient cohort, I started looking into both infective and inflammatory potential causations. So first thing that comes up as you all know is that the concept of infections presenting itself as a non-infectious disease. This is being discussed for many, many decades and at this moment in time, certainly recently, adult onset asthma now is being seen as a manifestation of a persistent infection. Interstitial cystitis is now seen more and more as being a persistent biofilm infection of the bladder. Certainly recurrent cystitis now is recognized as being a persistent infective disorder, irritable bowel, chronic sinusitis, gingivitis, periodontal disease. Recently there has been a finding of increased bacterial load present in women who either miscarried or had premature labour. Sarcoidosis has been implicated as being caused by bacterial infection. And macular degeneration with Chlamydia trachomatis as being a potential causative agent.
Now, we also find that there is a persistent inflammatory condition going on in my chronic pain patients and this is a recent quote from Nature, 2008, which basically describes this type of inflammation as a para-inflammation, which is expressed, arising from resident macrophage dysfunction.
Now, the other thing that’s been coming up again-–this is like Medicine, things go through cycles and the cycle now is this re-awakening of an interest in persistence in chronic infections. And this is again a recent publication where it states the various aspects of bacteria, both in their nature as well as their ability to evade the immune system as becoming more and more recognized as a problem and in terms of bacteria we are now looking at and recognizing that they have a colony type of pattern and they also have foreign consciousness. And so that, you can almost think of them as like a bee hive. You got the worker bees, we’ve got the active bacteria. We’ve got bacteria in that same colony that are designated persister cells. And we also have part of the bacterial load that are in dormant or in very low metabolic rate. And the other thing that’s interesting is that it is being speculated that over 99 percent of all the species that are present in the environment fail to grow on laboratory medium. They also grow very slow, like Tuberculosis bacteria. And so, if you are looking for a pathogen in a urine, in a bladder infection, a chronic recurring urine bladder infection and you do 24 to 48 hour culture you may not pick up any significant colony growth and you will have a report coming back that you have no infection. Also because the adaptive immune system is not functioning very well, it’s more an inflammatory condition, that same urinalysis will come back negative for leukocytes.
Now, this is really following up in terms of Dr. Marshall’s presentation. So, there I am. I’m a clinician, I have a significant number of people who are not functioning very well. Who are dependent on medications that are not very effective and have significant side effects and adverse effects. And in terms of some of the more recent drugs, the biologicals, have a significant economic load on their finances.
So, in researching this out, this hypothesis that Dr. Marshall has stated which I have learned about, about five years ago, and that hypothesis was: was there a possibility that one of the ways that bacteria persist in the body, is that it’s able to sabotage the innate immune responseThe body's first line of defense against intracellular and other pathogens. According to the Marshall Pathogenesis the innate immune system becomes disabled as patients develop chronic disease. and because, interestingly enough, there seems to be a pathological calcification component to a lot of these conditions and relates to Vitamin D metabolism and now as we know the nuclear VDR is very important in terms of innate immune response, that this VDR could become hypo-responsive through some mechanism that the bacteria has learned how to do.
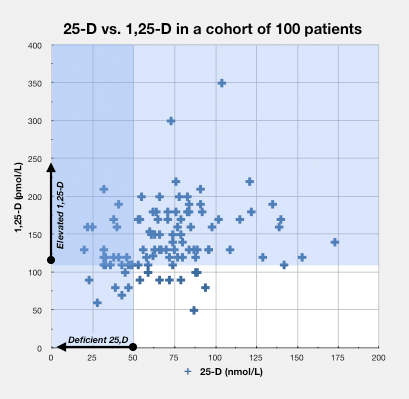
So I did my own unfunded study, which is: I took a hundred of my patients and the breakdown was basically, out of that hundred three of them were documented autoimmune diseases, 42 of them were chronic fatigue syndrome (fybromyalgia) and the rest were some metabolic syndrome and there was some, it was called post treatment Lyme Disease syndrome, patients, basically people who have had some event where they were infected with a zoonotic infection that was treated or not treated and had persistent symptoms afterwards. And what I did is, I basically measured their serum levels for 25-hydroxy vitamin D, 1,25-dihydoxy vitamin D, CRP which is a phase 1 protein, CK which I have found in my interest in muscle skeletal medicine was often elevated and ferritin.
And what I found was, is that the most sensitive or the most consistent finding was a finding of an elevation of the 1,25-dihydroxy vitamin D. I used the cut off point of 110 pmol per liter. If you want to convert that into American terminology feel free to divide by 2.4. And I used that level because that is kind of the consensus as the high normal for 1,25-D. Some researchers have put it at 130 which is when you‘ll start seeing hypercalcemia but in my… there’s not a lot out there in terms of normal values of 1,25-dihydroxy D but that was the best that I came up with. And the ranges were anywhere from 110 up to 350 pmols per liter, which is exceptionally high, with no hypercalcemia, interestingly enough.
The 25-hydroxy vitamin-D which I put as deficiency at less then 50 nmols, which I think is a pretty well and agreed upon determination of deficiency state. Only 26 of those 100 patients had that finding, with a range between 20 and 49 nmols per liter.
CRP was positive in 17 out of the 100 patients. Elevated CK was positive in about 12, and elevated ferritin was positive in only 4 of that 100 patients.
So, interpretation, well interpretation was–is that elevated levels of 1,25 dihydroxy Vitamin D above 110 was a pretty sensitive and consistent indicator of–in this small cohort of patients with autoimmune disease and autoimmune-associated diseases–at the time I did this, chronic fatigue syndrome was not seen as an autoimmune type disease while there was certainly evidence for suggesting that there was altered immunity, but it was not put into that category, it now is.
And this does suggest the fact that there is a presence of the Vitamin D receptorA nuclear receptor located throughout the body that plays a key role in the innate immune response. hypo-responsiveness. And again, I’m a clinician, the one that stands out for me is type 2 diabetes where there is an increased resistance to insulin and one of the manifestations of that is an elevation in insulin levels in the early phases of type 2 diabetes and it’s only later–even if it does occur–where the insulin levels start dropping, which interestingly enough is what we find in some of our chronic patients with chronic disease that we are talking about.
So, again, “clinician,” I went, well if this is the case, maybe we should try and do something about their condition and use a treatment. And so, using the information developed by Dr. Marshall and also doing the research into the angiotensin receptor blockers and how they are now being increasingly used for non-antihypertensive conditions such as rheumatoid arthritis where they are using 10mg per kilogram levels of Valsartan in one study, also being used in research in terms of metastatic cancer, again in 10mg per kilogram dosages, with no toxic effects. So we used Olmesartan because of molecular modeling information as well as patient response. We used Olmesartan even though you can use some of the other ARBA drug which is an angiotensin receptor blocker. One of the ARBs is olmesartan (Benicar). Not all ARBs activate the Vitamin D Receptor.’s and we used them in dosages of 40mg in every 6 to 8 hours. And with the main intention of reducing angiotensin II pro-inflammatory cytokinesAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system., which are implicated in a lot of these conditions such as atherosclerosis and many of those co-morbid conditions. It also, as indicated by modeling, has a VDR-agonistic effect and this is confirmed clinically because that when you use Olmesartan in a significant number of patients they show symptoms of immune activation which we call immunopathology and sometimes will even express to the point where it will be very similar to IRIS, so-called Immune Reconstitution Inflammatory Syndrome that is seen in AIDS-patients with high dose HAART.
Then we went at the infective component, we used bacteriostatic antibiotics of a variety of type. We initiate with one of them initially and then, after we built up to a certain level of dosage with that, we add a second. Clindamycin in particular is interesting because it has an amplification effect of other antibiotics when given in concert with other antibiotics. We start with fairly significant low dosages: 25mg minocycline typically every 48 hours. Azithromycin we start with 25mg every 10 days. The reason for that is, as you know, Azithromycin has a very long half life–60 hours–and has very good tissue penetration and stays in the tissues for a long time. The intention of using these low dose sub inhibitory levels of antibiotics is to reduce the bacterial virulence factors. Again this is something that has been shown in the research, that if you use low dose antibiotics you don’t kill the bacteria and therefore you don’t induce resistance or dormancy or persister cells but you do reduce the ability of them to avoid the immune system response and to persist. It also, we’ve used it in a pulsed manner because in that way there is not a consistent environment of antibiotic concentrations, which again will have a tendency to effectively reduce the development of mutant resistant strains and at dosages that obviously are very low or no toxicity.
I’m going to go real quick in a couple of case histories. This is a 52 year old male with multiple sclerosis diagnosed 1995, wheel chair bound. Initial assessment: his 25-DThe vitamin D metabolite widely (and erroneously) considered best indicator of vitamin D "deficiency." Inactivates the Vitamin D Nuclear Receptor. Produced by hydroxylation of vitamin D3 in the liver. was 79. His 1,25-D was 120. Interestingly enough he had an IgG, antibody level of 1 to 320 for bartonella henselae and we initiated the therapy so that roughly a year and a half later he was on full dose of minocycline-clindamycin and his 25-D was now into 50 and his reduction of his 1,25.. and his bartonella levels went to 64.
We then continued the protocol of that period of time. He had a significant reduced 25-D at that time but at the same time clinically was better. And then we checked him again in 2007, he was starting to go to more normal pattern of 25-D and 1,25-D which is persistent.
Second case is a 30 year old female chronic fatigue for six years, positive ANA at the Mayo clinic. She was also positive for IgM, Western Blot Borellia. Again you’ll see that her 25-D was not below 50. She was 94. She had a 160 1,25-D. She also had an evidence of being exposed to rickettsia with no past history of rickettsial infection. She then started to see the same pattern of the 25-D going towards a certain 50 to 60 pattern and the 1,25 dropping below 110.
What is interesting in 2008 is that she was continuing to improve symptom wise but her 1,25 all of a sudden shut up to 200 and this is an expression of this delayed increased immune response that we can characterize as similar to an IRIS pattern, but she became ANA negative.
Then the last one is chronic fatigue syndrome. This one I just want to identify in terms of the questioning 25-D levels as being assumption of Vitamin D storage. We assessed her in August of 2007, her 25-D level was 138 nmols per liter. She had elevated CRP, she had an elevated ferritin and she had an elevated IgG for Anaplasma. Then in December 2007, no therapy initiated, she was down to 96 / 130 still elevated therapy, then we initiated Olmesartan only and there her 25-D was now down to 65.
So, basically this is what we has observed. With Olmesartan alone we had pretty reliable reduction of 1,25 levels, we have improved symptomatology with 50 percent of the patients we had increased with 10 percent. Then when we add the antibiotics we get aggravation of symptoms through immunopathological response and then later increased inflammatory response. But as treatments progressed the Vitamin D metabolites would tend to normalize down to 25-D between 50 and 70 and 1,25 between 50 and 90.
So, summary: to say 1,25 Vitamin D is a sensitive clinical marker of an autoimmune in chronic disease and reflects para-inflammation and VDR hypo-responsiveness. This para-inflammation could be due to persistent bacterial infection both because of what I have found serologically and also what we have found in response to ant-bacterial medication. Pro-inflammatory cytokines can be safely reduced with ARB’s. Sub inhibitory levels of bacteriostatic antibiotics are effective in reducing bacterial burden. And finally, resolution of the inflammatory condition is reflected in the normalization of Vitamin D metabolites.
Thank you.