Related article: Immune Suppression

Table of Contents
Palliative vs. curative treatments
Introduction
Many first-line treatments for chronic disease were developed before it was understood that the death of chronic bacteria necessarily results in an immunopathological response and temporary feelings of malaise. Such treatments are designed to slow the immune response under the mistaken premise that autoimmune disease results when the immune system attacks the body.
According to the Marshall Pathogenesis, bacteria drive chronic disease, and treatments that slow the immune system only appear to “work” because they decrease bacterial death. While this causes a drop in inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue. that offers temporary symptomatic relief, bacteria which drive the disease state cease to be targeted and spread easily. The net result is that patients generally become increasingly ill over the long-term.
In essence, feeling better is not the same as getting better.
Anything which makes you feel better, almost always does so because it is stopping the immune system from killing the pathogens. The reason patients remain ill is that one just cannot apply the standard logic of “feeling well” to these chronic diseases. You have to understand the disease mechanism.
Trevor Marshall, PhD
In contrast, treatments that target the root cause of an illness rather than masking symptoms are curative in nature. While patients taking curative treatments may not always feel better during the course of therapy, such treatments have the potential to bring about lasting recovery.
Nevertheless, because palliative treatments that slow immune function are very effective at offering temporary relief, the number of medications, over-the-counter supplements, and fortified foods that work by slowing the immune response have escalated over the past decades. Since the goal of every Marshall Protocol (MP) patient is to effectively target the bacteria making them ill, such immunosuppressants must be avoided. These immunosuppressants range from corticosteroidsA first-line treatment for a number of diseases. Corticosteroids work by slowing the innate immune response. This provides some patients with temporary symptom palliation but exacerbates the disease over the long-term by allowing chronic pathogens to proliferate. and TNF-alphaA cytokine critical for effective immune surveillance and is required for proper proliferation and function of immune cells. blocking medications to “vitamin” D.
Common sources of palliation
Those substances that aim to cover up disease symptoms but do not succeed at reversing the disease state are palliative in nature. A variety of commonly taken medications, foods, and supplements offer temporary palliation by depressing immune function.
We surgeons have been operating on the gut for literally thousands of years and the microbiotaThe bacterial community which causes chronic diseases - one which almost certainly includes multiple species and bacterial forms. has just been this extraordinary elephant in the room. We seem to have completely ignored the fact that we've co-evolved with thousands of bacteria over millions of years and that they somehow may be important to our health. As doctors, we routinely do terrible things to the microbiota and I'm sure this has implications for our health.
James Kinross, Imperial College of London at 2008 International Conference on Metagenomics
Medications
Related article: Non-MP medications
The following is an incomplete list of medications that are immunosuppressive:
- TNF-alpha blockers – Tumor necrosis factor-alpha or TNF-alpha is a cytokine critical for effective immune surveillance. Anti-TNF drugs, also known as TNF-alpha blockers, are drugs which interfere with the body's production of TNF-alpha.
- telmisartan - This ARBA drug which is an angiotensin receptor blocker. One of the ARBs is olmesartan (Benicar). Not all ARBs activate the Vitamin D Receptor. is a VDR antagonistA substance such as 25-D or certain bacterial ligands which inactivates the Vitamin D Receptor the receptor which transcribes the genes necessary for a proper innate immune response. (has the opposite action to olmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. , which is a VDR agonistA substance such as olmesartan (Benicar) or 1,25-D which activates the Vitamin D Receptor and transcribes the genes necessary for a proper innate immune response.). It is a very strong immune suppressant.
- interferon – Interferon therapy is immunosuppressive, reducing in number both cytokinesAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. and immune cells.
- corticosteroids – Patients with chronic disease may find that while taking corticosteroids, both symptoms and markers of the disease such X-rays or liver enzymes temporarily decrease. However, according to a comparative study1), 74% of patients relapse a significantly higher percentage of the time after trying to ease up their Prednisone, the first-line treatment for a number of chronic diseases, and:
Relapse… rarely occurred in patients who had not been treated with corticosteroids in the past. The striking difference in relapse rate between treated and untreated patients suggests that patients with disease that would later be severe and protracted were almost unerringly identified early in their course…. Corticosteroids contribute to the prolongation of the disease by delaying resolution.
Jonathan E. Gottlieb et al.
Foods and supplements
Related articles: Food and drink, Non-MP over-the-counter supplements
The almost inevitable gravitation towards foods and supplements that slow immune activity (and diminish a bacterial die-off reaction) appears to be done subconsciously by people who play host to significant numbers of chronic bacteria. These foods and supplements include:
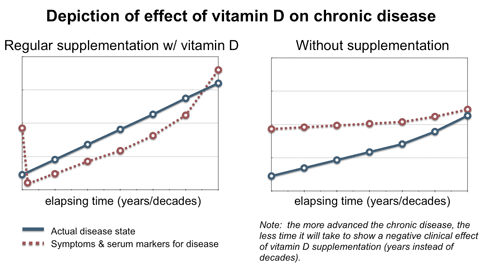
- vitamin D – Emerging molecular evidence suggests that symptomatic improvements among those administered vitamin D is the result of its ability to temper bacterial-induced inflammation by slowing VDRThe Vitamin D Receptor. A nuclear receptor located throughout the body that plays a key role in the innate immune response. activity.
- soy – Soy contains phytoestrogens such as genistein, which act directly to inhibit innate immune function.
- coffee – Coffee contains chlorogenic acidAn antioxidant and phenolic compound which in ways that are not yet fully clear can modulate and/or suppress the immune response, an antioxidant and phenolic compound, which, in ways that are not yet fully clear, can suppress the immune response. Frequent consumers of coffee often point to caffeine as giving coffee its addictive quality, but the role of chlorogenic acid offers another way that coffee can offer temporary symptom relief.
- fish oil – In addition to containing high amounts of vitamin D, supplemental fish oil contains the omega 3 fatty acids, several of which have been shown to interfere with production of TNF-alpha, an important cytokineAny of various protein molecules secreted by cells of the immune system that serve to regulate the immune system. necessary for the response of the innate immune system.2)
Marshall Protocol patients are generally advised to avoid supplements and to consume any food in moderation. Additionally, MP patients should try to get any vitamin through whole foods.
The Marshall Protocol is a curative treatment
The Marshall Protocol (MP) is a curative therapy and represents an alternative to therapies which mask or delay symptoms of disease. The MP aims to target the Th1 PathogensThe community of bacterial pathogens which cause chronic inflammatory disease - one which almost certainly includes multiple species and bacterial forms., which we now believe are ultimately responsible for chronic inflammatory disease.
One cannot judge the success of any therapy in the treatment of chronic illness by symptomatic improvement over the short term.
Greg Blaney, MD
Related publications and presentations
[PMID: 9118698] [DOI: 10.1378/chest.111.3.623]
[PMID: 18063921]

