Presentation - Bacteria induced vitamin D receptor dysfunction in autoimmune disease: theoretical and practical implications for interpretation of serum vitamin D metabolite levels
Presenter: Capt. Tom Perez MPH
Conference: 6th International Congress on Autoimmunity
Location: Porto, Portugal
Date: September 11, 2008
See also:
Transcript and slides; Notes from the 2008 International Congress on Autoimmunity by Amy Proal; More study results
Transcript
I will focus my presentation on the data and measures of response to the Marshall Protocol which I will refer to as The Protocol for short. First I would like to start by sharing with you the concepts underlying The Protocol.
As both Trevor Marshall and Greg Blaney have discussed previously, both dietary vitamin D and its metabolite 25-hydroxyvitamin-D (25-D) are secosteroids and Vitamin D Receptor (VDR) antagonists. Acting much like corticosteroids, as they reach higher levels in the body they block the proper operation of the innate immune system and thus prevent the body from mounting an adequate defensive response to pathogens. Certain intracellular bacteria also are able to cripple the innate immune system by blocking VDR functions. The result is a gradual increase in the body’s load of microbial pathogens, leading to a wide range of chronic autoimmune and inflammatory diseases.
We find that restoration of VDR function is essential to recovery from these diseases. Since supplementing vitamin D is counter-productive for the reasons mentioned earlier, we use olmesartan, a VDR agonist, to begin to activate the VDR and to restore innate immune function.
The use of olmesartan, combined with low doses of carefully selected bacteriostatic antibiotics, help to gradually restore VDR function by assisting the immune system in eliminating the bacteria that block the VDR. Bacteriostatic antibiotics interfere with the bacterial defense mechanisms and other processes crucial to bacterial survival.
Immunopathology or IP is a term used to describe an immune response which results in damage to the cells and tissues of the body. We generally see it as inflammation, and we experience it with a variety of symptoms that are typically associated with Autoimmune Disease.
The Protocol treatment triggers cycles of immunopathology that provide confirmation that an individual, in fact, has Th1 disease.
Infected individuals given dosage levels olmesartan adequate to begin activation of the VDR and a starting dose of 25 mg of minocycline every other day produce a measured IP response to each dose.
It should be noted that immunopathology is not reported in normal healthy individuals who are treated with antibiotics. This is why patients without the signal levels of D metabolites or with symptoms of chronic disease often trial a therapeutic probe to provide a clinician with an indication of Th1 disease and suitability of using The Protocol for treatment of their disease. Immunopathology provides a Measure of Treatment Response and Progress. Over time a particular dosage level of antibiotic produces less and less IP. When little to no IP is evident the patient progresses to the next recommended dosage level or if the highest recommended dose has been reached they progress to the next Protocol antibiotic.
The change in antibiotics will similarly produce IP. Therefore, it is imperative that the same cautions and specific ramping of dosages be followed throughout The Protocol.
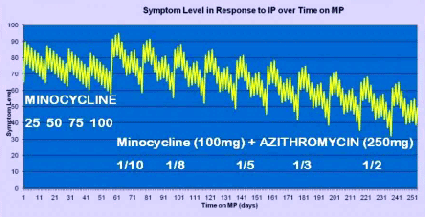
This slide illustrates the typical IP response that can be experienced by a patient. Initially the symptom level often increases above what the patient was experiencing prior to the beginning of treatment.
During the first phase of treatment, IP increases when the minocycline reaches optimal serum levels and then drops off before the next pulse of antibiotics. Each time the IP stabilizes, the dose is increased until a patient is ready for the second phase.
Later, the IP is in response to more than one antibiotic and is less regular in its pattern of intensity. I'd like to point out that the dose of azithromycin is initiated at a dose of 25-31mg every 10 days.
Immunopathology is generally predictable over the course of treatment with a trajectory of less and less IP experienced as the disease process is reversed, resulting in recovery. Thus, the eventual absence of IP provides a measurable primary endpoint.
This chart provides a cross-sectional, retrospective snapshot of 100 subjects sampled from our large observational Phase II Study that includes over 1000 individuals, of which approximately 550 are active participants.
The results in the slide are based on frequent progress reports and questionnaires. A more complete retrospective analysis will occur when future funding becomes available.
Our cohort includes many who are desperately ill. The average duration of symptoms for this group of patients is 19 years. Many in the cohort had unsuccessfully tried a variety of other approaches, including immunosuppressants prior to initiating The Protocol.
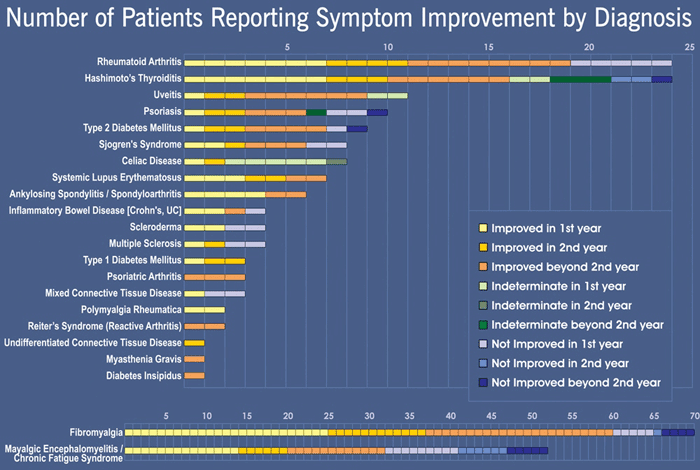
There are three main categories of treatment response in this graph: Those who improved first year, second year, beyond second year; those that were indeterminate in the first year, second year, beyond second year; and those not improved in the first year, second year, and beyond second year. Different shades of color in each of these categories tell us how long the patient has been on The Protocol.
As you can see rheumatoid arthritis and Hashimoto's thyroiditis are the largest groups by diagnosis, followed by uveitis, and psoriasis. Of the 12 patients with RA currently in their first year of treatment, 7 are improved and 5 are not improved. All RA patients beyond their first year of treatment have had improvement in their RA symptoms. (OK, you can compare the colors to follow them.)
For Hashimoto's Thyroiditis 7 of the 9 in their 1st year of treatment are improved and 2 are indeterminate. 3 of the 5 patients in their second year and 6 out of the 10 beyond their second year are improved. 3 patients beyond their 2nd year are indeterminate. And finally, 2 in their second year and 1 beyond the second year are not improved. These might be considered treatment failures, or they may need more time on The Protocol.
Th1 illness is typically characterized as one of many autoimmune diseases that develop over many years or decades. We have found that antibiotic therapy takes several years or more to induce full remission in these diseases.
…for patients who have currently been on The Protocol less than 18 months, 49% reported symptom level improvement all of the time, even during peak levels of IP, and of those who have been on The Protocol between 18 and 53 months, 81% reported improved symptom levels all the time.
The bar chart shows us that a lot of very sick people, with a lot of different diseases, have improved using the same treatment approach. We looked at the rate of improvement over time and found that for patients who have currently been on The Protocol less than 18 months, 49% reported symptom level improvement all of the time, even during peak levels of IP, and of those who have been on The Protocol between 18 and 53 months, 81% reported improved symptom levels all the time.
The Protocol medications are chosen for their effectiveness in supporting the immune system’s defense of the body against pleomorphic intracellular bacteria. The killing of these bacteria by the immune system always elicits an inflammatory cytokine release from the cells that they have parasitized. This results in a temporary exacerbation of inflammation and disease symptoms. Usually these symptoms are merely unpleasant, but they can be debilitating and even life threatening if care is not taken to cautiously follow The Protocol guidelines.
When taken at a dose of 40 mg every 6 hours olmesartan partially blocks the production of inflammatory cytokines by blocking the angiotensin II type 1 receptors and also affects additional receptors that influence inflammation, for example PPAR-gamma. This inhibits the release of TNF-alpha, and other cytokines involved in the Th1 immune reaction. Without the protection that olmesartan provides, patients experiencing severe IP may suffer tissue damage from this inflammatory reaction.
The other key role of olmesartan is to activate the VDR, which is especially important at the beginning of The Protocol, when the blockage of the VDR by bacterial pathogens is at its highest. This chart comes from Sankyo Pharma, New Drug Application to the FDA for olmesartan medoxomil. As you can see, the majority of olmesartan’s hypotensive effect is achieved with a dose of 20 mg and very little additional hypotensive effect occurs as the dose is increased beyond the 20 mg.
The success of this treatment Protocol is vitally dependent on using olmesartan at higher than hypertensive doses. A dose of 40 mg every 6 to 8 hours is necessary to assure adequate protection from damage that could be caused by inflammation during IP and to activate the innate immune system’s functions provided by the VDR.
Thank you.
I leave you with these take home points.
And I do have a small number of handouts for anyone interested.