Main article: Birth control

Table of Contents
Pregnancy, fertility, and menopause
Both olmesartan (Benicar)Medication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. and minocycline, the two mainstay medications of the MP, are contraindicated during pregnancy and while breastfeeding. When used in pregnancy during the second and third trimesters, drugs that act directly on the renin-angiotensin system can cause injury and even death to the developing fetus.
When pregnancy is detected in women on the MP, they must discontinue olmesartan (Benicar) as soon as possible. Also, minocycline hydrochloride, like other tetracycline-class antibiotics, can cause fetal harm when administered to a pregnant woman.
Women who are contemplating pregnancy should consult with their physicians about treating inflammatory disease first. Women with inflammatory disease who are already pregnant should do everything possible to keep the level of 1,25-DPrimary biologically active vitamin D hormone. Activates the vitamin D nuclear receptor. Produced by hydroxylation of 25-D. Also known as 1,25-dihydroxycholecalciferol, 1,25-hydroxyvitamin D and calcitirol. down. This means diligent avoidance of ingested vitamin D and exposure to sunlight/bright lights.
Fathering children while on the MP
A man on the MP may be able to father children with a healthy female, however, bacteria causing Th1 diseaseAny of the chronic inflammatory diseases caused by bacterial pathogens. can be transmitted during sexual contact and are transmissible to an ovum and/or a fetus.
MP may restore fertility
For 60 years, doctors have believed women were born with all the eggs they'll ever have. Recently Harvard scientists are challenging that dogma, saying they've discovered the ovaries of young women harbor very rare stem cells capable of producing new eggs.1) This work suggests that formation of oocytes is driven by the biochemical environment, as is all stem cell activity.
The MP is a curative therapy. As the MP resolves inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue., this healing will likely restore sexual capability and fertility. Any or all aspects of the MP, including avoiding vitamin D and sunlight/bright lights, may contribute to hormonal changes which lead to restoration of health and fertility in men or women.
Therefore, women of childbearing age on the MP should take adequate precautions to avoid getting pregnant. Women using contraceptive medication should consult with their health care practitioners at each phase of the MP about any possible reduction in effectivity that may be caused by the use of low-dose, pulsed antibiotics.
One of the MP cohort had been infertile for 15 years, but became pregnant at age 45, 6 months after starting the MP. She stopped to deliver and wean the baby and is now back on the MP.
Trevor Marshall, PhD
Birth control
Related articles: Pregnancy and fertility, Female hormone supplementation
Women of childbearing age on the MP who do not want to risk the chance of bearing a child suffering from fetal or neonatal injury should take precautions to prevent pregnancy, as the FDA package insert lists these as complications of taking olmesartanMedication taken regularly by patients on the Marshall Protocol for its ability to activate the Vitamin D Receptor. Also known by the trade name Benicar. during the second or third trimesters. According to the FDA, these adverse effects do not appear to have resulted from intrauterine drug exposure that has occurred only during the first trimester.
Because the MP can increase or restore fertility, women of childbearing age who are on the MP and sexually active are advised to use adequate precautions to avoid getting pregnant.
The doses of hormones found in birth control are low enough that patients need not be excessively concerned with their effect on immune function.
Pregnancy and disease
Pregnancy increases 1,25-D
Main article: Pregnancy and vitamin D
Production of 1,25-D is increased during pregnancy and may lead to disease exacerbation.
Pre-term delivery
Microbes play an important factor in whether a woman will carry a pregnancy to term.
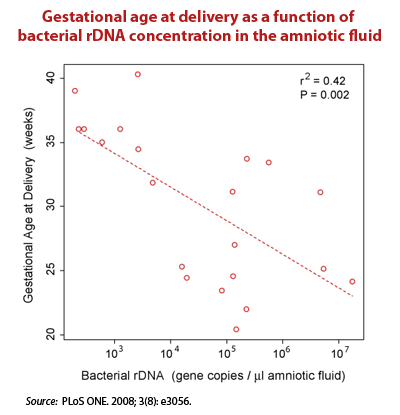
Using molecular tools to quantify bacterial count in pregnant women's amniotic fluid, DiGiulio et al. showed that the number of bacterial sequences found was inversely correlated with length of pregnancy.2)
Also underscoring the importance of microbes in premature delivery is a 2010 paper showing that the injection of lipopolysaccharides (endotoxins) could create a mouse model for preterm labor.3) The release of endotoxins are well known byproducts of the immunopathological response, which is generated when gram-negative bacteria are destroyed.
In recent years, the incidence of preterm deliveries has increased in the U.S. The National Center for Health Statistics (Centers for Disease Control and Prevention) has reported a 20% increase (from 10.6% to 12.7%) in the percentage of preterm deliveries during the years 1990–2005.4)
Sarcoidosis
The following describes some of the effects of sarcoidosis on pregnancy:
- Women with sarcoidosis report feeling better when they are pregnant. Sarcoidosis involves a Th1-activated immune system response. The NF-kappaBA protein that stimulates the release of inflammatory cytokines in response to infection/IkappaB signaling pathway is down-regulated in T cells in pregnancy, shifting the immune system away from Th1 and toward a Th2 immune response.5) There are other factors to consider, especially vitamin D and sunlight exposure. These play a role in activation of NF-kappaB and the Th1 immune response.
- Pregnancy in women with sarcoidosis usually goes to term with no problems. Pregnant women diagnosed with sarcoidosis need to be aware, however, that some of the drug therapies (methotrexate, anti-malarials, Thalidomide, etc.) normally used for sarcoidosis are contraindicated in pregnancy. 6)
- Oral corticosteroidsA first-line treatment for a number of diseases. Corticosteroids work by slowing the innate immune response. This provides some patients with temporary symptom palliation but exacerbates the disease over the long-term by allowing chronic pathogens to proliferate. increase the risk of cleft palate.7)
- Regarding cesarian section versus vaginal delivery, consider that sarcoidosis inflammation is known to have an affinity for scar tissue.
Other chronic inflammatory diseases seem to exert similar harmful effects.
Risk of pre-term birth for expectant mothers taking multivitamins
Regular multivitamin-mineral supplement use during pregnancy, in a developed country setting, is not associated with size at birth. However, a 2010 study of British women found that daily multivitamin use in the third trimester was associated with preterm birth.8)
Vaginal microbiome fluctuates through menstrual cycle
Santiago et al. collected swabs of vaginal microflora from 17 women over the course of two consecutive menstrual cycles. Researchers noted a rise in Gram positive cocci during menses.9)
Patients experiences
I'm 54 years old and haven't had a period in two years and then had one in February. I am getting symptoms off and on of an impending cycle. Good thing I had my tubes tied years ago.
JudyBeauty
Related publications and presentations
[PMID: 22844256] [PMCID: 3406006] [DOI: 10.1371/journal.pgen.1002848]
[PMID: 18725970] [PMCID: 2516597] [DOI: 10.1371/journal.pone.0003056]
[PMID: 19995880] [DOI: 10.1093/molehr/gap106]
[PMID: 18772340] [PMCID: 2543075] [DOI: 10.2353/ajpath.2008.080257]
[PMID: 15034076] [DOI: 10.4049/jimmunol.172.7.4583]
[PMID: 10637902]
[PMID: 11091360] [DOI: 10.1002/1096-9926(200012)62:6<385::AID-TERA5>3.0.CO;2-Z]
[PMID: 20353456] [PMCID: 2874518] [DOI: 10.1111/j.1471-0528.2010.02549.x]
[PMID: 22140538] [PMCID: 3227645] [DOI: 10.1371/journal.pone.0028180]

