
Table of Contents
Alzheimer's disease and dementia
Meaning “deprived of mind,” dementia is a serious loss of cognitive ability in a previously unimpaired person, beyond what might be expected from normal aging. Alzheimer's disease – also called Alzheimer disease, Senile Dementia of the Alzheimer Type (SDAT) or simply Alzheimer's – is the most common form of dementia.
Recent evidence suggests that infectious agents need serious investigation as potentially important factors that contribute to the progression, complexity and severity of Alzheimer's.1) Perhaps the most striking of this evidence is that amyloid-beta, the protein which builds up in the brains of Alzheimer's patients, is an antimicrobial petide.
Diagnosis
Physicians use the diagnosis of mild cognitive impairment (MCI) to predict which patients have the highest risk of Alzheimer's. Although the rate at which patients go on to develop probable Alzheimer’s disease is relatively high – approximately 10-15% per year2) – the criteria for diagnosis of MCI excludes a lot of patients. In order to be given a diagnosis of MCI, patients must be “in good health,” have “no significant cerebrovascular disease,” and be between 55 and 90.3) These criteria rule out a number of patients sick with chronic disease. In fact, most patients with chronic disease report some level of cognitive dysfunctionThe loss of intellectual functions such as reasoning; memory loss; and other neurological abilities that is severe enough to interfere with daily functioning. and would otherwise easily meet the other criteria for MCI. Furthermore, normal cognitive performance is expected to decline as people age; also, people over 90 are ineligible to be diagnosed with MCI, because any memory loss over that age is expected.
In the clinical setting, Alzheimer's disease is usually diagnosed from the patient history, collateral history from relatives, and clinical observations, based on the presence of characteristic neurological and neuropsychological features and the absence of alternative conditions. Advanced medical imaging with computed tomography (CT) or magnetic resonance imaging (MRI), and with single photon emission computed tomography (SPECT) or positron emission tomography (PET) can be used to help exclude other cerebral pathology or subtypes of dementia. Definitive diagnosis of AD requires histopathologic examination, which is rarely done in life.
Evidence of infectious cause
- Amyloid-beta, the protein which builds up in the brains of Alzheimer's patients, is an antimicrobial peptide. – See following section
We are excited that someone [the team of Harvard researchers who first identified amyloid beta as an antimicrobial petide] is thinking out of the box in ways that others haven't considered. Most of the evidence about infections and AD has been ignored. The Harvard researchers are going about this in a rational way. It's not such a radical idea. HIV can trigger dementia. Why not other organisms?
Brian Balin, PhD, NeurologyToday
- Bacteria have already been shown to cause dementia and a corresponding deposit of amyloid proteins in a kind of syphilis – It has been known for a century that dementia, brain atrophy and amyloidosis (deposit of amyloid proteins in organs or tissues) can be caused by chronic bacterial infections, namely by Treponema pallidum in the atrophic form of general paresis in syphilis.4)
- Caregivers are more likely to get sick – A subject whose spouse experienced incident dementia onset had a six times greater risk for incident dementia as subjects whose spouses were dementia free.5) The article on familial aggregationOccurrence of a given trait shared by members of a family (or community) that cannot be readily accounted for by chance. discussed the transmissionAn incident in which an infectious disease is transmitted. of microbes and diseases at greater length.
- “Peripheral” infections can hasten the onset and progression of Alzheimer's6) – Cognitive function can be impaired for at least two months after the (apparent) resolution of a systemic infection.7) A 1999 study looked at 22 sets of twins, at least one of whom had been diagnosed with Alzheimer's. Five study participants had serious systemic infection developed Alzheimer's, and they tended to have earlier onset than their corresponding twin.8)
- Peripherally Applied Aβ-Containing Inoculates Induce Cerebral β-Amyloidosis - Intraperitoneal inoculation with β-amyloid–rich extracts induced β-amyloidosis in the brains of β-amyloid precursor protein transgenic mice after prolonged incubation times, possibly indicating that bacteria were co-transported in the extracts.9)
- Classic markers of inflammationThe complex biological response of vascular tissues to harmful stimuli such as pathogens or damaged cells. It is a protective attempt by the organism to remove the injurious stimuli as well as initiate the healing process for the tissue. are upregulated in Alzheimer's10) – Local brain tissue inflammation in Alzheimer's has been reported to involve upregulated production of classical inflammatory mediators of innate immunityThe body's first line of defense against intracellular and other pathogens. According to the Marshall Pathogenesis the innate immune system becomes disabled as patients develop chronic disease. such as tumour necrosis factor-alpha (TNF-alphaA cytokine critical for effective immune surveillance and is required for proper proliferation and function of immune cells.), interleukin 1 alpha/beta (IL-1 alpha/beta), interleukin 6 (IL-6) and complement proteins that are synthesised locally by cells in the brains of Alzheimer’s patients.11) 12) 13) Some anti-inflammatory therapies have been shown to temporarily delay the progression of Alzheimer's.14)
Specific pathogens already implicated in Alzheimer's
While many more pathogens will likely be identified in patients with Alzheimer's, certain easily cultured and readily identifiable microbes have been repeatedly identified in people with such conditions. According to Urosevic and Martins,15) these include the following viruses: herpes simplex virus 1 (HSV1), human immunodeficiency virus (HIV),16) hepatitis C virus (HCV),17) 18) human herpesvirus 6, cytomegalovirus and others.19) 20)
Strong evidence is available for the presence of intracellular bacterium Chlamydia pneumoniae in brains of AD patients.21) 22) In humans, C. pneumnoiae has been shown to reach the central nervous system via infected mononuclear cells following the breach of blood-brain barrier23) 24) and to induce Alzheimer's-like amyloid deposits in mouse brain upon injection.25) 26)
Finally, infection with Helicobacter pylori has been shown to lead to mild cognitive impairment and may therefore play a role in more severe forms of dementia.27)
Amyloid proteins, the hallmark of Alzheimer's, are produced in response to infection
According to the “amyloid hypothesis,” the lifelong buildup of amyloid-beta (amyloid-β) proteins in the brain is the precipitating factor of Alzheimer's disease.28) 29) Researchers showed that amyloid builds up in the brain before symptoms arise suggesting this hypothesis was true. Further confirmation for this explanation seemed to be offered by the fact that people with Down Syndrome – who have an extra copy of the amyloid beta precursor protein on chromosome 21 – almost universally develop Alzheimer's before the age of 40.30)
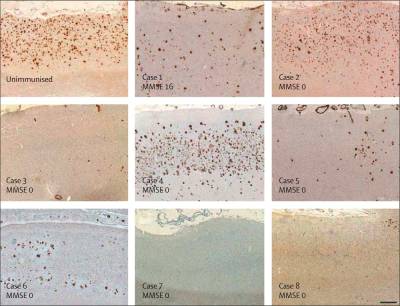
At this point, it seemed logical that stopping the production of amyloid-beta would also halt the cognitive decline associated with amyloid buildup. However, in a 2008 Lancet paper, Holmes et al. reported a trial in which an experimental vaccine succeeded in reducing production of amyloids (and the deposition of amyloids in the brain) but had no effect on neurological decline.31) This suggested that while amyloid deposits were associated with the disease, they did not cause it.
In a seminal 2010 study, a team of Harvard researchers showed that amyloid beta can act as an antimicrobial peptide, having antimicrobial activity against eight common microorganisms, including Streptococcus, Staphylococcus aureus, and Listeria.32) This led study author Rudolph E. Tanzi, PhD to conclude that amyloid beta is “the brain's protector.”
The similarities between Abeta [amyloid beta] and antimicrobials had been staring us in the face for decades. Abeta looks in size, structure, and biochemical properties like an antimicrobial peptide [called LL-37]. In fact, we have shown that it is a bonafide antimicrobial peptide.
Rudolph E. Tanzi, PhD, NeurologyToday
If amyloid beta were an antimicrobial, one would expect that suppressing amyloid beta production suppresses innate immunity. Indeed, one study found that genetically modified mice that lack the proteases needed to generate amyloid beta have a 60 percent neonate mortality unless raised in sterile conditions. Notably, four major markers of adaptive immune function were normal in these mice.33) A second finding comes from a clinical study of the drug tarenflurbil, published in 2009 in the Journal of the American Medical Association that was shown to slightly lower amyloid beta production. Most telling is that a side effect of patients taking tarenflurbil is significantly increased rates of infection.34)
Role of the Vitamin D Receptor
According to the Marshall PathogenesisA description for how chronic inflammatory diseases originate and develop., microbes subvert immune activity by suppressing expression of key nuclear receptorsIntracellular receptor proteins that bind to hydrophobic signal molecules (such as steroid and thyroid hormones) or intracellular metabolites and are thus activated to bind to specific DNA sequences which affect transcription. involved in innate immune activity such as the Vitamin D ReceptorA nuclear receptor located throughout the body that plays a key role in the innate immune response.. The fact that over-production of amyloid suppresses the VDRThe Vitamin D Receptor. A nuclear receptor located throughout the body that plays a key role in the innate immune response. suggests a role of VDR dysfunction in the Alzheimer's disease process. Indeed, a 2010 study in Journal of Alzheimer's Disease showed that the amyloids trigger neurodegeneration not only by inducing LVSCC A1C expression and NGF levels, but also by dramatically suppressing VDR expression.35)
Roles of Brain Angiotensin II in Cognitive Function and Dementia. 36)
Immune suppression
The most serious health endpoints that have been reported to be associated with extremely low frequency (ELF) and/or radiofrequency radiation (RFR) include childhood and adult leukemia, childhood and adult brain tumors, and increased risk of the neurodegenerative diseases, Alzheimer’s and amyotrophic lateral sclerosis (ALS).
Is the Marshall Protocol applicable for dementia patients?
Int J Cardiol. 2016 Oct: ACEIs and ARBs may effectively prevent all-cause dementia, particularly VD, in patients with type 2 DM and hypertension. Moreover, compared with ACEIs, ARBs appear to be more advantageous in dementia prevention. 37)
There is a clinic in Germany which is treating dementia with a variation of the MP and has found the patients herx to indicate a Th1 diseaseAny of the chronic inflammatory diseases caused by bacterial pathogens.. However, by the time the disease becomes advanced, they are no longer able to look after themselves, and the MP requires a lot of self-discipline in order to be effective.
The problem is compliance, as the patients have trouble focusing on avoiding sunlight/Vit-D, and remembering to take their Benicar. They seem to be responding. And, most important, they herx, their disease relapses after a day soaking in the sun, and some show (very) tentative signs of recovery.
There is not much to be gained by varying from the base MP. With the dementia patients it is tough to get 100% compliance, unless they have an efficient caregiver (in other words, they don't take their meds on time). Additionally, there is little appreciation, at the level of the patient, of avoiding ingested Vitamin D.
There is little chance that a patient having gone through the MP is likely to develop dementia, but at this point it is also unlikely that Alzheimer's patients, in an advanced state of disease, would be able to discipline themselves enough for recovery.
Trevor Marshall, PhD
Published in AJH February 2017 ARB protects Alheimer's
Shuko Takeda & Ryuichi Morishita Angiotensin Receptor Blocker protects Alzheimer's Disease Brain from Ischemic Insult
Role of lifestyle factors
A 2011 study used a mathematical model to surmise that modifiable conditions such as physical inactivity, smoking, depression, low education, hypertension, obesity and diabetes are responsible for about half of the roughly 5.3 million Alzheimer’s cases in the United States and 34 million cases worldwide.38) They went on to conclude that reducing the prevalence of these risk factors by 10 percent could prevent 1.1 million cases worldwide; reducing these risk factors by 25 percent, they claimed, could prevent more than three million cases.
This study fails to consider that such “lifestyle choices” may be due to other factors entirely. A patient with artificially controlled hypertension or diabetes or is a patient who smokes and is unable to quit is not the same as a healthy patient.
Other antimicrobial therapies
Epidemiology and costs to society
Alzheimer’s disease affects approximately 4.5 million people in the U.S. and this number will increase as the population ages and the life-span increases. It is projected in 50 years, as the population ages and the life-span increases, AD will afflict approximately 14 million people.41) Two-thirds of nursing home residents have dementias.42)
Dementia, and specifically Alzheimer's disease, may be among the most costly diseases for society in Europe and the United States,43) the greatest of which is long-term healthcare. Numbers vary between studies but dementia costs worldwide have been calculated around $160 billion,44) while costs of Alzheimer in the United States may be $100 billion each year.45)
Read More
[PMID: 18487850] [DOI: 10.3233/jad-2008-13407]
[PMID: 14732621] [DOI: 10.1001/archneur.61.1.59]
[PMID: 18487847] [DOI: 10.3233/jad-2008-13404]
[PMID: 12754353] [PMCID: 1738504] [DOI: 10.1136/jnnp.74.6.788]
[PMID: 10026389] [DOI: 10.1159/000017115]
[PMID: 20966215] [PMCID: 3233904] [DOI: 10.1126/science.1194516]
[PMID: 8866675] [DOI: 10.1016/0165-0173(95)00011-9]
[PMID: 11754986] [DOI: 10.1016/s0197-4580(01)00289-5]
[PMID: 12476347] [DOI: 10.1080/13550280290100969]
[PMID: 14962152] [DOI: 10.1111/j.1532-5415.2004.52109.x]
[PMID: 9771753] [DOI: 10.1038/2677]
[PMID: 12614463] [DOI: 10.1046/j.1365-2893.2003.00416.x]
[PMID: 11826420] [DOI: 10.1053/jhep.2002.30688]
[PMID: 16240484] [DOI: 10.1017/s104161020500195x]
[PMID: 12875814] [DOI: 10.1016/s0966-842x(03)00146-x]
[PMID: 20182626] [PMCID: 2825657] [DOI: 10.1155/2010/273573]
[PMID: 9749980] [DOI: 10.1007/s004300050071]
[PMID: 12584732] [DOI: 10.1002/jnr.10519]
[PMID: 10024578] [PMCID: 96464] [DOI: 10.1128/IAI.67.3.1323-1330.1999]
[PMID: 15013562] [DOI: 10.1016/S0197-4580(03)00127-1]
[PMID: 17581756] [PMCID: 2039821] [DOI: 10.1007/s00401-007-0252-3]
[PMID: 17718688] [DOI: 10.1111/j.1468-1331.2007.01827.x]
[PMID: 1763432] [DOI: 10.1016/0165-6147(91)90609-v]
[PMID: 19096156] [PMCID: 2615484] [DOI: 10.3233/jad-2008-15404]
[PMID: 16904243] [PMCID: 3375834] [DOI: 10.1016/j.neurobiolaging.2006.06.023]
[PMID: 18640458] [DOI: 10.1016/S0140-6736(08)61075-2]
[PMID: 20209079] [PMCID: 2831066] [DOI: 10.1371/journal.pone.0009505]
[PMID: 20009055] [PMCID: 2902875] [DOI: 10.1001/jama.2009.1866]
[PMID: 20966550] [DOI: 10.3233/JAD-2010-101377]
[PMID: 23304450] [PMCID: 3529904] [DOI: 10.1155/2012/169649]
[PMID: 27390970] [DOI: 10.1016/j.ijcard.2016.06.215]
[PMID: 21775213] [PMCID: 3647614] [DOI: 10.1016/S1474-4422(11)70072-2]
[PMID: 19240960] [DOI: 10.1007/s00415-009-5011-z]
[PMID: 18487851] [DOI: 10.3233/jad-2008-13408]
[PMID: 15685097] [DOI: 10.1016/s0755-4982(05)83882-5]
[PMID: 16401889] [DOI: 10.1159/000090733]
[PMID: 9543467]

