Related article: Diseases associated with low levels of 25-D

Mistaking correlation for causation in vitamin D studies
Many vitamin D studies suffer from methodological errors including bias inherent to using self-selected subjects and insufficient followup, but perhaps their most egregious liability comes in mistaking correlation for causation. 1)
It's undisputed that a wide array of studies point to the fact that 25-hydroxyvitamin D (25-D) – typically referred to in the media as vitamin D – is low in people with numerous chronic inflammatory diseases. However, these studies fail to prove that low 25-D causes disease. Even so, some studies assume that doubling serum levels of 25-D would drastically reduce mortality.2)
In fact, molecular science has revealed that the levels of the vitamin D metabolites through a series of intricate and carefully controlled feedback pathways, mechanisms that belie the simplistic first-order mass-action model used to guide the short-sighted vitamin studies. Also, epidemiological evidence suggests that while 25-D is low in chronic disease, 1,25-D (1,25-dihydroxyvitamin D) tends to be very high, an observation which is at odds with the theory that vitamin D deficiency causes or exacerbates disease.
There have been lots of observational studied showing an association between various diseases and vitamin D deficiency, but there is not any evidence yet that that is a casual relationship… it may be that vitamin D deficiency is a marker of ill health.
Dr. Ruth McQuillan, University of Edinburgh
Causation is not self-evident
There are a number of examples where low levels of a substance are known to be associated with but not cause disease.
- Folic acid – Low levels of folic acid often lead to an increase in the amino acid homocysteine – a compound that at high levels has been linked to increased incidence of cardiovascular disease (CVD). Yet, extensive studies have revealed that giving patients with CVD folic acid supplements does not lower levels of homocysteine, and that high levels of homocysteine in patients with CVD is simply a result of the disease process.3)
- Estradiol – In a recent study, both low and high serum levels of estradiol (a type of sex hormone), compared with mid-range levels, are significantly and independently associated with increased all-cause mortality in men with chronic systolic heart failure.4) Yet, lead author Dr. Ewa Jankowska would quickly dismiss the idea that supplementation with estradiol reduces the risk of heart failure.
Of course, the study does not suggest that low and high estradiol concentrations themselves were the cause of increased mortality.
Vasan Ramachandran, MD, Heartwire
Even among those who support widespread supplementation with vitamin D on the basis of the “deficiency” studies, there is wide acknowledgement that the understanding of vitamin D metabolism is “imprecise.”5)
Causation should never be assumed to be self-evident.6) Rigorous analysis is required, especially for a system as complicated as vitamin D metabolism.
Actually, there is no experience of causation: events do not wear their causal credentials on their faces.
L.R. Karhausen 7)
In the absence of an understanding grounded in molecular and clinical evidence, the comprehension of how vitamin D affects disease becomes “black box epidemiology.” 8)
As suggestive as any set of data might seem, absent a precise understanding of underlying disease mechanisms, researchers could just as well conclude, for example, that:
- all pain conditions is a deficiency of opiates, since narcotic pain medications activate opiate receptors in the brain
- fever is caused by too little aspirin
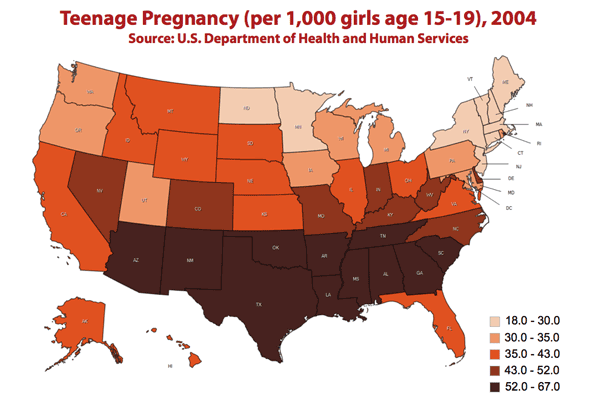
- sunshine exposure causes teenage pregnancy
Researchers should also measure 1,25-D
Related article: Evidence for high 1,25-D in patients with chronic disease
Most published epidemiological research looking at levels of vitamin D in those with chronic diseases fail to note any measure of 1,25-D, a metabolite which is often elevated in those with chronic disease. Dr. Greg Blaney, a physician who practices in Vancouver, British Columbia (a setting with relatively infrequent sunlight), found that of a group of 100 patients with a variety of chronic inflammatory diseases, 85 had elevated measures of 1,25-D, which was defined as greater than or equal to 110 pmol/L.
The practice of failing to measure 1,25-D is pervasive: the NIH continues to accept studies and a number of journals continue to publish papers.
Further, mistaking 1,25-D for other forms is more common than one might think. A 2011 study actually gave “cholecalciferol” but called it elsewhere “1,25-dihydroxyvitamin-D.”9)
One of the reasons that 1,25-D isn't measured may be that it is harder to test. But another reason may be that a high 1,25-D is inconsistent with reports of vitamin D “deficiency.” How can patients be said to be “deficient” in vitamin D when one of its metabolites, 1,25-D, is often several standard deviations greater than normal?
“The idea that widespread vitamin D deficiency exists in the world has never had any credibility, and the idea that vigorous supplementation is necessary therefore has to be false.”
“Nowadays it is virtually impossible to buy milk in the US that has not been laced (‘fortified’) with vitamin D. The amounts added, and the content, have been subject to dubious control, and a number of fatalities have occurred due to Vitamin D poisoning from milk.”
“The mis-labeling of this compound as a vitamin is regrettable, as it gave a potential toxin an aura of undeserved innocence. Vitamin D is not a vitamin, but a steroid, which is, in its most active form, a powerful hormone with receptors widely distributed in the tissues of the body. As with other steroids, excessive consumption has risks.” Dr Hywel Davies
[PMID: 27610068] [PMCID: 5003588]
[PMID: 21731036] [DOI: 10.1038/ejcn.2011.68]
[PMID: 17309931] [DOI: 10.1161/CIRCULATIONAHA.106.686238]
[PMID: 19436016] [DOI: 10.1001/jama.2009.639]
[PMID: 17867374] [DOI: 10.1111/j.1753-4887.2007.tb00344.x]
[PMID: 11080970] [DOI: 10.1023/a:1009970730507]
[PMID: 22004229] [DOI: 10.1111/j.1756-185X.2011.01684.x]